- Raymond, or Life and Death
Over the years I’ve read many books and watched many videos about mediumship, near death experiences and the like, but never quite let go of the scepticism instilled by my conventional upbringing and scientific education. I recently asked Claude AI to recommend some serious books on the subject, and one of those on the list turned out to be among the most remarkable I have ever read. Raymond, or Life and Death by Sir Oliver Lodge was published in 1916 and is a long book in three parts: a memoir about World War One, an extensive investigation of mediumship, and a discussion about what might be called consciousness studies. The author was an Englishman, a brilliant physicist and electrical engineer whose research into electromagnetic radiation contributed to the development of radio. He and his wife lived in the Birmingham suburb of Edgbaston, incidentally the place where I was born. They had twelve children and the youngest, Raymond, is the subject of the book.
Raymond, like his father and brothers, was a highly intelligent man with a passion for engineering. He was also by all accounts a very pleasant and thoughtful person whom everybody liked. When war broke out he volunteered to serve as an officer in the British Army and after a short training period was deployed to a secret location on the Western Front. His duties involved the design and construction of trenches and dugouts, and he was also trained to operate machine guns. His letters home are reproduced in full and though perhaps they put a positive slant on things he writes that he is happy and cheerful and even enjoying parts of the experience, despite the deaths and mental breakdowns of some of his comrades. I found it interesting and moving to read this detailed account of what life was like for these young men on the front line. After a few months he was struck by a German shell and died an hour or so later. He was 26 years old. Numerous tributes from his relatives, colleagues and friends are reproduced in the book.
Oliver Lodge had already been involved in the Spiritualist movement, along with other eminent men of his time such as Arthur Conan Doyle. Very soon after learning of Raymond’s death, Lodge and his wife scheduled sittings with several different mediums, taking elaborate precautions to safeguard their anonymity. The early communications reported that Raymond had felt confused at first but was now happy in the afterlife, surrounded by many friends, and keen to come through to bring comfort to bereaved relatives on earth. General information of this kind might have been either genuine or fabricated, and in later sittings Lodge sought for more specific evidence. The first of many examples came from a detailed description of a photo of Raymond and his comrades, taken shortly before Raymond died. Lodge did not know about this photo until he was able to obtain a copy later, which rules out telepathy as the explanation. Many other sittings with various mediums provided convincing evidence of Raymond’s survival. Special techniques such as automatic writing and table tilting were sometimes used, and if Lodge had lived 100 years later he would no doubt have taken part in the current research which is using modern technology including AI.
The last part of the book called “Life and Death” draws on philosophy, biology, physics and the author’s own theories. I didn’t understand it all, but had the impression that our understanding of consciousness, mind-body-spirit connections and an afterlife has not changed all that much today. Lodge stresses the importance of keeping an open mind, being willing to revise firmly held beliefs and to admit the limitations of current scientific knowledge.
- Historical psychiatric biographies
To accompany my husband’s recently published autobiography A Psychiatrist’s Journey, I’ve posted a list of loosely related books on the website formerly known as Shepherd, now called BookDNA.

Of course I had to include the classic biography of Sigmund Freud by Ernest Jones. This is an admirable work but so long that neither Brian or I ever got through it. In the section of his autobiography that describes his sea voyage from New Zealand to England, where he was to begin psychiatric training at the Maudsley Hospital in London, Brian wrote: “I took Ernest Jones’ three volume biography of Freud, thinking it an appropriate introduction to psychoanalysis. I started to read it several times but could not get far before I started to yawn.”
To see the other books I selected – all of which I did read and enjoy, though they might not be ones that Brian would have chosen – please click here:
https://bookdna.com/best-books/historical-psychiatric-biographies
- Thoughts on preparing for widow(er)hood
I’ve written this post in the form of an advice column, in the light of my experience following the death of my husband Brian. Nothing can take away the anguish of losing a beloved partner, but things can be done over the preceding months and years to make it easier to cope when the time comes. Some of this advice may sound very obvious but is often neglected.
- Don’t put off talking with your partner about what will happen after one of you dies, upsetting though such conversations may be. It can be easy to avoid the topic when you are young and fit and assume you will live for years to come. But if you wait too long it may be too late for meaningful discussion because of illness, deafness, confusion or extreme old age.
- Keep your finances and online presence in order. Besides making a will, write more detailed document(s) including such things as your wishes for end of life care, funeral arrangements, a list of your accounts with official bodies and social media platforms even if you don’t want to reveal full access, and any other information that will make it easier to settle your estate. These documents can be stored securely with a lawyer and/or family member. Update them every few years.
- Be prepared to take over each other’s roles. There are still some traditional marriages in which the man never learned to cook and the woman never learned to drive. I was already dealing with the everyday running of our own household and its finances, but am not mechanically minded and have needed help with some quite simple practical tasks that I used to leave to Brian.
- Declutter from time to time. A burdensome aspect of dealing with Brian’s estate, also with my mother’s estate ten years earlier, was going through multiple boxes containing papers like old bank statements, and personal documents which were not meant for me to read. It felt disloyal to throw such things away, but few of them needed to be kept and I disposed of the majority by hiring a large “secure document destruction bin”.
- Keep some selected physical items such as items of clothing, letters, cards, photos and videos. Looking back at photos of Brian, and of the two of us together, continues to be tremendously important to me and I have printed out some of the digital ones to keep in a special album. Electronic records are not a substitute for tangible keepsakes, and they can be lost.
- However close the relationship, maintain some friendships and interests that can be carried out independently of your partner. Brian didn’t join me in choral singing or dog walking, but I have continued these activities and the social contact has been very helpful in coping with bereavement. In contrast some of the things we used to do together, like going to Waiheke Island for lunch, are not much fun on either my own or with someone else.
- Don’t leave important things said or questions unasked. Even if the intense early romance has passed, keep telling your partner that you love them.
- “A Psychiatrist’s Journey” by Brian Barraclough

Following the death of my husband Brian, the task of editing the memoir that he had asked me to complete has been a bittersweet experience. His book has now been published under the title A Psychiatrist’s Journey and is available in ebook or print versions from many online retailers: https://books2read.com/u/4NzOJN.
A long detailed account of Brian’s varied and productive life, it’s not intended for a wide commercial market but should appeal to people with an interest in the history of medicine and psychiatry, those who grew up in 1930s Auckland, and those who knew him personally. Taking over this project, which was so important to Brian, has been a big responsibility and I hope I’ve done it justice.
I left the wording almost exactly unchanged, resisting any temptation to add things in or take things out, except where clarification was needed or information was repeated. My main change involved reorganising the document into shorter sections, adding headings to make it easier to read and to navigate. It needed many minor copy edits such as standardising the use of capital letters and the format of abbreviations. I made some use of tools like “search and replace”, but they can introduce errors and anyway it was a labour of love which I preferred to do myself by hand. I did employ help with the layout and illustrations from a colleague who has worked with me on previous books. I didn’t use AI.
A short blurb:
“A candid memoir by Brian Barraclough (1933-2025), best known for his research on psychiatric and social aspects of suicide. His book covers growing up in New Zealand, having tuberculosis aged 17, training as a doctor at the University of Otago, practising general medicine in Christchurch and psychiatry in Dunedin before sailing to England as a ship’s surgeon. He worked at the Maudsley Hospital in London, the Medical Research Council unit in Chichester, and the University of Southampton before retiring back to Auckland. His book describes many memorable patients and colleagues and his wide leisure interests including art, European travel, and medical history.”
Here again is the link where you can read a preview: https://books2read.com/u/4NzOJN.
- “Book marketing experts”
The first time I received an unsolicited email containing fulsome praise for my recently published novel, and a proposed marketing plan, I felt quite flattered and impressed. I replied explaining that due to personal circumstances I didn’t want to proceed at present but would be interested at a later date. Almost at once another email came, this time including a detailed script for a YouTube trailer about my book. It seemed too good to be true, and my suspicion grew when I googled the sender and found nothing about a book promotion service under their name. Even so, in my naivety it took me a while to realise that my correspondent was an AI.
Since then I’ve received many other emails offering to market either my latest book or a previous one. They lavished compliments on my writing: “the work of someone who deeply understands human relationships, subtle suspense and the power of memory and place” “the story breathes psychological nuance, clarity and compassion” “you illuminate the hidden layers of human conflict, emotion and resilience”.
Some of them did appear to come from a real person, although it was hard to tell, and maybe would have led to a genuine marketing campaign if I had taken them up. But I suspect others were from scammers who might take my payment and never contact me again, or even hijack my financial details for illegal purposes. I will never find out, because I am getting tired of the growing influx of such emails, and have started deleting them unread.
- My first weeks of widowhood
Brian was 14 years older than me and had a history of heart disease, so we knew it was likely that he would die first. I tried to prepare myself for the event but it was impossible to predict when and how it would happen, or how I would feel afterwards. Much has been written about coping with spousal bereavement but everyone is different and there is no right way to respond to this monumental life experience.
There have been many practical and administrative matters to deal with during these first few weeks. I have had wonderful support from family, friends and former colleagues, being showered with flowers and food and invitations to meals, cards and letters expressing condolences for me and appreciation for Brian. Although my grief is profound I have not been overwhelmed by it, but have managed everything efficiently and kept in good health. Christmas preparations and festivities are underway too, so I have been very busy. I don’t know whether that is a good thing. I’m afraid that after Christmas, when all the activity and attention has wound down, the loneliness and boredom of being without Brian is really going to sink in.
Brian and I had a wonderful life together until the last few months when the nature of his illness prevented any meaningful conversation between us, and made it unsafe for him to be nursed at home where he longed to be. He had very good care in the hospital, and I did all I could to support him there, but his distress could not be relieved and he wanted to die. Thankfully his last 24 hours were peaceful.
I have a few regrets. I wish that when he was still well we had talked more about planning the future, done some decluttering and possibly downsized. And, although it is comforting to look through all my photos of Brian, I wish I had taken more videos of him.
- Brian Barraclough 1933-2025
My beloved husband Brian died from respiratory failure last week.
He was 92 years old and in recent months had endured a gruelling decline of both body and mind, due to cardiac and cerebrovascular disease. He was ready to leave this world and while it is a blessing that his suffering is over, his death is a great loss for me. During the 47 years we were together my role had gradually evolved through different stages – mistress, wife, nurse and now widow. Of course there were challenges, but not too many. We had a wonderful marriage.
There is much else to be thankful for. Brian had excellent care from the staff of North Shore Hospital in Auckland. I am receiving a huge amount of support, especially from Brian’s three nieces, and from friends and relatives in both New Zealand and the UK. My cats are being especially affectionate at night.
We will have a small private funeral service, then I expect there will be a difficult few months ahead, sorting out Brian’s affairs and possessions, adjusting to life without him, and doing my best to develop a happy future for myself.
Brian had not quite finished writing his extended autobiography. Due to his incredibly vivid and detailed memory, the document contains a lot of valuable information not only about his own life but about the history of psychiatry in both NZ and the UK. I aim to complete the editing process and publish it next year.
- Hospital days
My husband Brian is in hospital. Over recent months he’s been developing a complex, fluctuating mix of physical and mental symptoms. He has been very ill and spent about two weeks on a medical ward before being transferred to a unit for older people, where he is improving, and benefiting from activities – both of us took part in a bowling match (!) and have taken trips to the beach.

My days have taken on a new pattern – in between spending long hours with Brian at the hospital dealing with the house and garden, the cats, my own healthcare appointments, responding to emails and texts. I’ve continued my exercise classes and choir practice, but otherwise am not doing much. There’s no time for socialising and I lack the concentration for any serious reading, writing or other constructive activity. But I am coping better than I did during the similar stressful period ten years ago when Brian had major cardiac surgery and I developed a range of stress-related problems (I described that experience on this blog and in a short book).
We hear a lot of complaints about New Zealand’s hospitals in the media, but Brian has had excellent treatment. The kindness and patience of the staff, including especially the health care assistants, has been wonderful. I hope Brian will be well enough to come back home soon, so we can pick up the threads of our previous life, and it will be important to complete and publish his new book about his long medical career.
- Novels about the psychology of marriage
Here’s my list of “The best novels about the psychology of marriage” on Shepherd.com. It includes five books on a theme loosely related to that of my own new novel. Most of the plots involve some kind of marital conflict, or touch on the related topics of adultery, widowhood and divorce, but have (reasonably) happy endings.

This is the third list I’ve published with Shepherd. The process of compiling them encourages me to read more widely and reflectively, as well as providing a stress-free method of publicising my own books.
I dislike promoting my own work. I sometimes feel physically sick when writing emails to friends and acquaintances to tell them about my latest book. I’ve had little success with paid adverts and promotions in the past, so I don’t do them any more. When I was younger I enjoyed giving talks, even to large audiences, but not any more. All the same, with around three million books now being published each year in the US alone, indie authors like myself have to do some marketing if they are going to achieve more than a handful of sales.
So, in the hope that you’ll have a look at No Good Deed, here is a comment emailed to me by one reader:
“My goodness your new book is incredibly powerful, backed up by strong writing. I couldn’t put it down and it affected me emotionally as well … I thought the climax was stunning.”
No Good Deed is available in print and ebook versions from major online retailers through this link.
- Music, spirituality and religion
Is a strong Christian faith essential for writing, performing or appreciating sacred church music? And how much does the music contribute to the spiritual experience of a church service?
I’ve been thinking about these questions since a recent visit to the cathedral which I used to attend regularly as a member of the choir. We sang mainly traditional classical pieces in four voice parts with organ accompaniment. On the day I returned, the organ was not being played and “my” old choir had been replaced by a youth group singing loud upbeat music. They were obviously well trained and enthusiastic and I expect many members of the congregation liked their modern style. But I found the sound more intrusive than uplifting. This confirmed that, for me, music is a vital part of a service.
The British composer John Rutter (born in 1945) would probably agree about this. He has spoken and written in some detail about his attitudes to religion and spirituality. He describes himself as an agnostic, who values the traditions of the Church of England but does not accept all of its doctrines. In one interview he spoke of understanding the universe in terms of a lottery governed by mathematics, rather than by an all-powerful deity. He said he believed in a more general sense of spirituality which can be accessed through the beauty of nature or art as well as through music.
I was curious to find out something about the beliefs of other men (they have all been men) whose choral sacred music I have enjoyed singing. According to the information I found online, some of the greatest classical composers – Bach, Mozart, Handel, Haydn – were devout practising Christians. In contrast, there were others who had been brought up in the Christian faith but had doubts in later life, leading them to explore wider concepts of spirituality. Beethoven was one of these, and more recent examples include Berlioz, Faure, Elgar and Vaughan Williams.
Whether or not they held a conventional religious faith, it seems that many of these men believed in an intangible realm beyond the material world as being the source of music. Having the ability to access this source is a wonderful gift, though inspiration is not enough on its own. The process of composing works that can be performed by other people requires a thorough knowledge of the technicalities of music, and a great deal of hard work.
A few quotes:
Beethoven: Music is the mediator between the spiritual and the sensual life.
Bach: I play the notes as they are written, but it is God who makes the music.
Vaughan Williams: There is no reason why an atheist could not write a good Mass.
Elgar: My idea is that there is music in the air, music all around us; the world is full of it, and you simply take as much as you require.
Haydn: When I think of my God, my heart dances within me for joy, and then my music has to dance too.
P.S. Since drafting this post I have visited London and heard glorious singing during a Latin Mass at St James, Spanish Place.

Image from WordPress Free Photo Library - Chartwell and Biggin Hill
While in England this summer I visited Chartwell, the home of Winston Churchill and his wife Clementine. I had wanted to go there for years but the house, situated deep in the Kent countryside, seemed too difficult to access without a car. Then I discovered that a bus from South Bromley goes there on Sundays.

Chartwell: Photo by Charlie Seaman on Unsplash The house contains many displays of Churchill memorabilia, and is furnished in a simple but elegant style reflecting Clementine’s taste. I especially liked her bedroom, painted in her favourite shade of duck-egg blue. Winston’s bedroom was not open to the public.

Lady Churchill’s room: Photo from National Trust 
Dining room: Photo by Jez Timms on Unsplash The extensive grounds include walled flower and vegetable gardens, ponds and woodlands. I didn’t find Churchill’s painting studio, but had seen many of his art works inside the house. Nor did I see Jock, the latest of the marmalade cats that have always been kept at Chartwell. All the same it was a very worthwhile visit.

One of the ponds at Chartwell Another place I’ve long wanted to see is the RAF museum at Biggin Hill, so it was a very nice surprise to find that the bus route went past it. I went in and was shown round the beautifully kept memorial chapel dedicated to the airmen who lost their lives in WW2. There was a separate display honouring the women who served as ferry pilots and in numerous ground roles.
From an adjacent site, it is possible (for a hefty price tag) to take a flight in a Spitfire. This is something else I’d love to do. Maybe next year …

Spitfire at Biggin Hill - My new novel
I’m pleased to announce the publication of my latest short novel No Good Deed.
“Charlotte and Henry’s quiet retirement is upended when a medical school reunion forces Charlotte to confront a long-buried trauma. Her search for closure takes a sinister turn, and meanwhile Henry’s heart condition is getting worse. A tragicomic tale with a chilling final twist.”
The old saying “No good deed goes unpunished” gave me the idea for this book, and the storyline evolved gradually over a year or two. Although it’s not directly autobiographical it draws on my experience as a medical student, practising doctor, patient, patient’s wife – and life coach. It touches on some serious themes but has humerous aspects too.
No Good Deed is available in ebook or print formats from multiple online retailers. Please have a look: https://books2read.com/u/b5Exvk.

- The art of the blog
My husband sometimes asks me why I write a blog. I usually reply “Because I like doing it”, which probably is the main reason but not the only one. For myself, it is a way of widening my knowledge and views about different subjects, and providing a record of significant events and aspects of my life. For readers, I hope it provides some information and entertainment. I’ve had many interesting comments, with no unpleasant ones so far, and made a few online friendships with people from around the world – a modern equivalent of “penpals”.
I started with Google Blogger many years ago, then changed to WordPress where I have published almost 300 posts. At one time I ran four separate blogs on specific subjects, but this system proved too cumbersome to manage so I put them together and my “category cloud” now includes a wide range:

I don’t have a huge readership but am satisfied with several hundred followers from different platforms, and a handful of visits every day always including archived posts, those about Bach flowers being most popular.
I only post when I have a new idea to write about, which is seldom more than once a month. Ideally I would like to post once a week, provided that I could come up with worthwhile content rather than cluttering up the internet with boring trivia or embarrassing personal details. Some of the people whose blogs I follow maintain a much more regular and frequent schedule, and I admire them. For example a new post from The Cricket Pages, by Rachel, arrives in my inbox at the same time every Sunday without fail. And The Mindful Migraine, by Linda, posted every single weekday for its first year and now three times a week. Both these blogs are always worth reading.
- Writing the blurb for a new novel
Writing a book – in my opinion – is much easier than marketing it. As stated in an article on Draft2Digital, crafting the blurb requires a switch from “author” mode to “copywriter” mode, which may not come naturally. Their recommended structure for a fiction blurb begins with a “hook”, and ends with “social proof” such as excerpts from reviews.
My own forthcoming novel No Good Deed is not directly autobiographical, but in keeping with the advice to “write about what you know” it draws on my own experiences ranging from sexual harassment at medical school, my husband’s heart attack, and on a lighter note life coaching and cookery. I’m currently working on the blurb, and here is a draft version. Any suggestions about how to make it more compelling would be welcome. I haven’t (yet) sought help from ChatGPT.
Marriage. Memories. Medicine. Poison.
Charlotte and Henry, a married couple in their sixties, live a comfortable but monotonous life somewhere in the English midlands. Henry recently retired from his post as a consultant pathologist at the local hospital. Charlotte once hoped for a medical career of her own, but following an experience of abuse during her student days she had a “nervous breakdown” and did not complete the course. She now combines being a homemaker with doing good works in the local community, although her efforts tend to misfire. She has recently started seeing a life coach who is encouraging her to be more assertive. When Henry insists that she accompanies him to a medical school reunion she attempts to confront her abuser, with sinister consequences. This tragicomic story ends with a dark twist.From Amazon reviews of Jennifer’s earlier novels:
You Yet Shall Die: I found the book both intriguing and unusual. I could hardly wait for the story to unfold as family secrets, crime and murder came to light – the ending was totally unexpected. An absorbing read.
Cardamine: This is a gripping mystery which keeps you guessing until the end, with twists and turns up to the last page.Three Novellas: Jennifer brings together all her experiences from previous work to produce a superb trilogy finishing with an interesting twist.

Photo by Debby Hudson on Unsplash - The Elgars in the Alps

Edward and Alice Elgar 1891 I’m now singing with the Harbour Voices choir on Auckland’s North Shore. Our next concert will include some songs from one of Edward Elgar’s lesser-known works, From the Bavarian Highlands (Op 27).
I’ve always loved Elgar’s music. In the long-ago days when I was a young single woman with an old-fashioned record player for company in the evenings, I repeatedly listened to the Cello Concerto, Enigma Variations, and the Pomp and Circumstance March No 1 better known as Land of Hope and Glory.
My interest in Elgar grew when I started visiting Malvern many years later. He was born in 1857 into a musical family living in the nearby village of Lower Broadheath. Their modest house is now a small National Trust museum called The Firs.

Elgar’s birthplace Elgar loved walking on the Malvern Hills, as I do, and perhaps it was the proximity of Alpine walks that led him and his wife Alice to spend a holiday in Garmisch, Upper Bavaria in 1894.

Garmisch Inspired by the lilting melodies of the folk songs and dances from the surrounding mountainous regions, the Elgars composed From the Bavarian Highlands between them. Edward wrote the music, in the form of songs for SATB voices with a piano accompaniment, and Alice wrote the lyrics. The Dance, with its tuneful joyful rhythms, is followed by the wistful False Love, the soothing Lullaby, and the gently spiritual Aspiration.
For any local readers of my blog who would like to attend the concert, here is the poster with the details.

- Recurring themes in fiction
Many fiction writers include similar characters, settings, plot lines and underlying themes in different books even if they are not part of a series. This may be deliberate, if they have already found a successful formula and want to give readers more of the same. At other times it happens less consciously, and reflects personal experience or psychology.
In my last post I wrote about entering my eligible novels, through Draft2Digital, into Apple’s trial of digitally narrated audiobooks. Cardamine was first to be published in this format, and Carmen’s Roses is now available too. These two books were originally written several years apart, and until I listened to the previews of their first chapters I hadn’t quite realised that they both begin with an Englishwoman taking a holiday in New Zealand. Not surprising really, because such holidays were a significant part of my own life before I moved permanently to Auckland. Cardamine and Carmen’s Roses are quite dissimilar otherwise although their plots both involve a missing woman. This is the case in some of my other writing too although I don’t know why. I also realise that several of my novels feature unpleasant male doctors. These characters are not based on any one real individual, but are informed by various interactions I have had during my own medical career and as a patient myself.
Cardamine, Carmen’s Roses and some of my other books can be found at https://books2read.com/jenniferbarraclough.

- The audiobook of Cardamine
I’m pleased to announce that my novel Cardamine: a New Zealand mystery is now available from Apple’s Audiobook Store.
Producing an audiobook in the traditional way, with the text read by live actors, is so expensive and time-consuming that I have never considered doing it. But I was recently invited through Draft2Digital to submit some of my fiction books for inclusion in Apple’s trial of using digital voices. It was free for me to take part, so I decided to accept.
Cardamine is set in New Zealand in the summer of 2019. Kate, on the last day of her backpacking holiday, loses her bag in a vineyard and misses her flight home to England. An eccentric elderly man comes to her rescue and invites her to stay on as his paid companion in his country home. The man’s wife is away, said to be back in her home country, but Kate comes to suspect that her absence has a more sinister explanation…
My digital voice, called Amberley, has a British accent appropriate for the character of Kate. She’s not very good at pronouncing Māori place names, but otherwise I think she does a good job of telling the story. I am interested to see that Apple has set the price at twice that of the e-book, even though it was presumably very cheap to produce, and it will be interesting to see if anyone buys it.
This book and some of my others others can be found at https://books2read.com/jenniferbarraclough

- A day without wine …
Some years ago, a local Italian restaurant displayed a placard reading “A day without wine is a day without sunshine”. That message would probably attract disappproval nowadays, when there are so many warnings about alcohol-related damage to health. While the risks and benefits of drinking continue to be disputed I continue to have a glass of wine with dinner on most evenings, though I intend to give it up for Lent.

Image from Unsplash In 2022 the World Health Organisation (WHO) published a statement in The Lancet to the effect that no level of alcohol consumption is safe, primarily because even small amounts can promote cancer growth. However many published studies have reported that light to moderate drinkers have lower mortality than teetotallers, and a reduced incidence of cardiovascular disease, diabetes and dementia. The research methods have sometimes been criticised and the evidence is conflicting. Perhaps it is too difficult to generalise because the effects of drinking vary so much between populations, and between individuals, depending on genetic makeup and lifestyle factors.
Heavy drinking is obviously harmful and people who are pregnant, have a history of alcoholism or of certain medical conditions are advised not to drink at all. But for those of us with no contraindications, any risks of light-to-moderate intake (up to 14 units a week) must be weighed against the benefits of pleasure, relaxation and sociability as well as possible cardiovascular protection. And the Mediterranean diet, widely recommended as a healthy eating pattern associated with longevity, includes red wine with meals.
After Easter I will go back to drinking wine, though not too much of it. As I get older I agree with the saying that one glass is medicine but two are poison.
***
On a different topic – nine of my ebooks are currently FREE in this year’s Smashwords sale. They are listed on the site https://books2read.com/jenniferbarraclough. Please note the promotion will end on March 8th, and only applies to the Smashwords versions – from other retailers they are still full price.
- Feline heartaches
I couldn’t stop crying when the time came to take our latest foster kitten, Nico, back to the rescue centre. We have fostered many kittens before and I have never been seriously upset about saying goodbye to them. Indeed it has been rewarding to see them grow in health and confidence while in our care, and be passed as ready for adoption. But Nico was somehow different.
He came to us at four months old, an unremarkable-looking tabby kitten, very thin because he had been suffering from bowel infections and presumably been malnourished in earlier life. He thrived while he was here, and quickly made himself at home, being let out of the foster room during the day if I was there to supervise him. He was energetic, playful and affectionate and he won our hearts.
We have two cats of our own, both 10 years old now. Leo, the male tabby, made friends with Nico right away. He enjoyed grooming him, and the two of them ate side by side.

Leo and Nico But Magic, our black and white female, reacted quite differently. She always knows when there are kittens here even when they are shut away in the foster room, and leaves the house for long periods, refusing to eat unless her meals are served outside. It has been worse this year and she has been completely absent from the property at times.
My husband Brian doesn’t usually get involved with the foster kittens, but he took to Nico so strongly that he suggested adopting him. We had long discussions about this. I wanted it too, because I had become so fond of Nico.But logically I knew it would be a mistake. I think we are too old to take on a young kitten who is likely to outlive us. Looking after three cats is a big commitment and expense. And a major barrier would be Magic’s mental health. Even now that Nico has been gone for several days, and I have given the foster room a thorough clean, she is reluctant to come into the house again. Al least she was back in our garden today, but didn’t take kindly to having her photo taken. “No good deed goes unpunished”, and by caring for foster kittens I have caused much heartache for Magic.

Magic Fostering is a lot of work and after doing it for a month, first for the two timid kittens and then for Nico, I am glad to have a rest and be free for other things. But I still miss Nico very much and do hope that he, along with all the many other cats and kittens currently in the shelter, will find the right forever home.
Update 5 days later: Nico has been adopted, and Magic has returned home.
- Kitten season

Photo courtesy of SPCA Auckland Every year during January, I volunteer to foster kittens from the SPCA. I clear the best furniture out of the dining room, which for the next few weeks becomes known as the foster room, filled with feeding bowls, litter trays, climbing frame and cat toys.
Kittens may require fostering for a variety of reasons. Some are healthy but still too young to be desexed and vaccinated prior to being adopted into forever homes. Some are recovering from an injury, or from illnesses such as cat flu and giardia. Others are frightened of human contact because they have been neglected or abused, and need a period of socialisation. And this year there are so many cats and kittens being brought in that the rescue centre is full to capacity, meaning that some animals need accommodating in private homes.
My current charges, a brother and sister about nine weeks old, were on anti-anxiety medication when they arrived. They were extremely timid, hiding in inaccessible places for much of the time, and it was very difficult to touch them. What a contrast to my previous kittens who have been desperate to escape from the foster room and explore. They did however seem physically healthy, eating and drinking well and have grown fast. Their confidence has gradually improved and now, two weeks later, they are lively and playful and purr loudly when stroked. I’m not allowed to post photos of them online, but they do look very attractive, with their white and tabby coats. It has been lovely to watch their transformation from frightened little kittens into thriving young cats.
Fostering requires quite a lot of time and effort. The least pleasant aspects are having to keep changing litter trays throughout the day, and the potential for damage such as torn curtains. It is also a bit hard on one of my own cats, who clearly dislikes having kittens in the house even though they are in a separate room. My other cat is quite happy to have them here.
These two kittens will be returning to the SPCA in a few days and will hopefully be adopted soon. I will miss them, but am going to exchange them for another litter which will bring new challenges and rewards.
- Cold showers, cemeteries and nomophobia
I’ve been exploring Modern Stoicism for a while now. Reading about the theory is easier than putting the ideas into practice, so this January I decided to subscribe to the New Year Challenge course run by dailystoic.com. It involves a series of assignments sent by email every day for 21 days. Most of them are not just one-off tasks, but are designed to introduce new habits to be continued long term. Some are practical, for example taking cold showers, doing pressups, and keeping to a regular bedtime. Others are more psychological, for example visiting a cemetery to aid the practice of memento mori, resuming a project that has been abandoned, and choosing a word to focus on all year – my word is PATIENCE.
Now half way through the course, I find some of the assignments easy because I am doing them already. But the challenge that I haven’t even tried to attempt is spending 24 hours without my iPhone. I do have some excuse, because I genuinely need it to deal with important messages throughout the day. But I have to admit to being quite addicted, and was absolutely devastated on the recent occasion when I thought it was lost (I found it some hours later under the duvet). I plan to compromise by spending a day without online games or social media, and even that will demand great self discipline. I obviously have symptoms of the condition popularly called “nomophobia” – fear of having no mobile.

- 2024
The year 2024 has brought mixed fortunes for me and husband Brian, with both pleasures and challenges. I’ve written this summary mainly for myself, but if you are interested please read on. Most of the topics mentioned have been covered in more detail in previous posts on this blog.
The first few months of 2024 were dominated by Brian’s medical issues. His artificial heart valve, inserted nine years ago, was failing and after a series of invasive tests he underwent a TAVI (trans aortic valve insertion) with a device similar to that pictured below.. The operation itself went well but was followed by two episodes of haemorrhage from the bowel, requiring emergency hospitalisations and multiple blood transfusions. Thankfully he has now recovered and, at the age of 91, is well and active. Modern cardiac surgery can achieve wonderful results.

After twenty-odd years as a member of the choir of St Patrick’s Cathedral, at Easter I made the difficult decision to resign. I loved singing in this setting, but the combination of Brian’s medical problems and the unreliability of the ferry service to central Auckland was preventing regular attendance. Also, since a few other long serving members had left, I realised I was 50 years older than almost everyone else! I have now joined a larger choir, Harbour Voices, which is nearer my home – and more appropriate to my age. Our three concerts this year have spanned a variety of musical styles and I’ve enjoyed singing in them.

As for my writing, my latest novel is slow going, but I’ve published some short reviews on the “Shepherd” site and one new book, Migraine and Me.

In September I spent two weeks in England, based in London and travelling round the country by train to see friends and family and favourite places. The photo below was taken on the Malvern Hills.

Since returning home there has been sadness with the deaths of three long-standing friends and colleagues, and stress with tenancy issues currently before the court. But on the whole life continues in a pleasant quiet routine, recently enlivened by the visit of Brian’s son, daughter and granddaughter from England. I keep reasonably fit with weekly TRX and Zumba classes, swimming in the warmer months, and daily walks with friends or one of my two “dog shares”, Ireland the Labrador and Buddy the Cavoodle.


Our two cats, Magic and Leo, are now ten years old and still in good health. Now that the New Zealand summer has arrived they spend a lot of time resting in the sun.

Happy Christmas and New Year, and thank you for reading my blog.
- Holiday reading recommendations
During this year I’ve read or reread a variety of books, and written brief reviews of some favourite ones for shepherd.com. If you’re wanting ideas either for your own reading over the holidays or for Christmas gifts, you might like to look at the lists below. Click on the images to see my personal appraisals of these books, with links to their details on your local Amazon site.
For my “Three favourite reads of 2024” – not necessarily published in 2024 – I chose three completely different books, one novel and two non-fiction:

My list of novels on the theme of “Family secrets and mysteries from the past” includes three modern classics which I’ve enjoyed reading again, and two contemporary psychological thrillers, linked to one of my own books:

Thirdly a non-fiction list on the theme of “Doctors who have been patients themselves“, including the short book about migraine that I published this year:

Seasons greetings to all my readers, and thank you for your interest in my blog and my books.
- AI for writers – wonders and dangers
An invitation to a free webinar about “AI for Authors” recently popped up in my inbox. Having little experience with AI, apart from using ChatGPT to generate an image for the cover of my last book, I watched the webinar with growing amazement. The presenter demonstrated how AI could write a story on a given topic with lightning speed, and then produce any number of edited versions with different prose styles or plot twists. He also showed how AI could generate content for a daily series of blog posts.
I am currently stuck with my new novel, which is loosely based on an episode of sexual harassment during my student days. I’ve written the first half but can’t decide how to continue the story towards a satisfactory ending. So as an experiment I asked ChatGPT for some ideas. With some apprehension, feeling rather as if I was sending in an essay likely to be criticised, I submitted a 500 word summary of the existing text.
The response came back at once. Following an introductory comment about “psychological conflict and unresolved trauma” it listed five possible directions in which the novel could develop. They were all appropriate, taking account of the story so far and the motivations of the four main characters. A human editor would have taken quite some time to read my summary and come up with so many options. I still find it incredible that AI could give such a detailed response instantaneously.
I could ask ChatGPT to give me more ideas, or even to finish the book for me, but I don’t intend to do so. Because I write mainly for my own satisfaction and enjoyment, it would seem pointless and a bit like cheating. AI must be an invaluable tool for certain professional writers, for example journalists working to a deadline. But over-reliance on AI, especially for fiction, could stifle originality and lead to the rapid churning out of books with recycled content and wide scope for plagiarism.
The awe-inspiring power of AI was predicted in a quote attributed to the late Stephen Hawking: ‘Somebody asks a computer “Is there a God?” and the computer replies “There is now”.’
Disclaimer: AI was not used in writing the text of this post. But I did ask ChatGPT for an image and received this reply:
“Here is the symbolic illustration representing the use of AI as a tool for writers. It highlights the harmony between creativity and technology. Let me know if you’d like any adjustments!”

- Family secrets and mysteries in fiction
Here’s my latest list of book recommendations, published through shepherd.com. It includes three modern classics which I’ve enjoyed rereading, and two more contemporary psychological thrillers. Have a look through this link: https://shepherd.com/best-books/family-secrets-and-mysteries-from-the-past.
- Revisiting my NZ/UK Trilogy
Except for those outstanding ones that acquire classic status, most modern novels lapse into obscurity within a few months of publication. This is a pity because they might well remain readable for years to come. The huge number of new books being released every day is one reason for declining sales. Another is a lack of ongoing marketing and, in common with many other authors, I feel uncomfortable with self-promotion. But there are times when it has to be done, so this post is about the revival of some of my earlier work.
Ten years have passed since I began my self-publishing career through Amazon kdp, with a short novel called Carmen’s Roses. Encouraged by its success I went on to write two sequels, Blue Moon for Bombers and The Windflower Vibration, published separately and then as a combined set called Three Novellas. To mark their 10th anniversary, and in the hope of reaching a wider readership, I am now reissuing them as low cost e-books on multiple channels through the Draft2Digital platform.

The first book Carmen’s Roses is set in Devonport, the Auckland suburb where I live. It is a story of mystery and romance which touches on some deeper themes. The narrator, Iris, is leaving the English winter to take a holiday in the New Zealand sunshine, with the intention of completing her recovery from a serious illness and making amends for a shameful episode in her past. But the shock of a sudden death, the shadow of an old love affair, and the onset of ominous new symptoms threaten to destroy her hopes of happiness and healing. The book, described by one reader as an “Interwoven tale of love, mystery and more than a touch of the paranormal'” received 5-star reviews on Amazon, for example “Jennifer draws believably on her medical background and in this story weaves a very tangled web indeed”.

The second book, Blue Moon for Bombers, is set in England in 2007, when an old man in his hospital bed is haunted by memories of serving with Bomber Command in World War Two. Meanwhile back in his country home, the continuing fallout from his wartime trauma leads to rising tension among the two younger couples who are marooned indoors by the summer floods. With testimony from an unexpected visitor, and some guidance from the spirit world, the family’s secrets are revealed and the emotional wounds begin to heal. Again, the reviews were positive: “Excellent strong plot … like a Victorian novel set in modern times” “Brilliant ending”.

Thirdly The Windflower Vibration, with action split between Takapuna in New Zealand and Malvern in England, continues and weaves together the stories from the first two books. A man dies while swimming off an Auckland beach, and a woman who witnesses the event becomes involved in its aftermath. Was the death due to natural causes hastened by medical malpractice? Or was it one strand in a complex web spread over two hemispheres and two centuries? Although I think this book is equal in standard to the previous ones it gained less attention, perhaps because it deals with characters in later life – just one 5 star rating, no reviews.
Rereading my three novellas recently I felt they deserved a new lease of life. So if you haven’t seen them before, please have a look at these ebooks, and some of my others, through this link. There are print versions on Amazon too.

- Memories of England in pictures
Twenty-four years after moving to New Zealand, I am very fortunate to still have many friends and relatives in England and still be able to go back and see them. A consecutive Britrail pass provides the freedom to travel around the country on any train at any time, to visit people and places that played an important part in my earlier life and to take some pictures to remember them by.
My mother was brought up in Ramsgate and Margate, and during my own childhood we often visited these and other seaside towns in Kent.

Broadstairs in the sunshine 
Folkestone harbour on a dull day My own childhood was spent in Gravesend. Returning there recently I found the town so changed that I hardly recognised it, and didn’t take any photos other than one of the house where I grew up.

Our old family home on The Overcliff Besides the outings to the seaside we often visited other parts of Kent.

North Kent marshes – where I set one of my novels 
Cutty Sark – now in Greenwich but was lying on the Greenhithe shore during my childhood My teenage years were spent in Yorkshire. I don’t often go back there now, but I took this picture during a delightful stay with an old school friend who lives in Wharfedale.

A stream near Leathley Oxford, where I attended medical school and spent most of my subsequent career, still feels like home. The city centre has deteriorated but walking by the river is lovely as ever.

River Thames in Grandpont Nature Park And a favourite place full of memories – the College of Healing course, the Elgar museum, the walks on the hills – is Great Malvern.

The Malvern Hills – I think this one is called the Sugarloaf 
Walking on the Malvern Hills A highlight of my time in London was a lunch party for 24 of the friends who have given me hospitality over the years.

One of three tables set for lunch As we all get older, and the state of the world gets more precarious, I know I may not see some of these people and places again. But I hope there will be more visits to England still to come.
- The best books by doctors who have been patients themselves
The website Shepherd.com offers readers a new way to discover books that may interest them. Each page describes one book by a contributing author, and five others on a related theme. I was invited to create a page on a theme of my choice, and having just published a memoir about my own migraine, I decided to look for books written by other doctors who had been patients themselves. I was less interested in the medical details than in the way the illness experience had shaped their personal and professional lives. I came up with a varied list of recommendations.
Doctors can face particular challenges when they become patients. The change of status may seem humiliating, as poignantly described in the saddest book on my list, by an eminent surgeon who felt himself reduced to “Just another old man with prostate cancer”. On the positive side, doctors who are still working may well become better clinicians especially as regards communication with patients and relatives. This comes through in a collection of vignettes about the everyday clinical work of a doctor with a long history of ulcerative colitis. A memoir by a medical student who was rendered quadriplegic in a car accident, but went on to qualify and build a successful career, is an inspiring read showing what determination can achieve. My two most unusual book choices are by doctors whose illness experience proved a catalyst for a move away from orthodox medicine towards alternative fields with a spiritual focus.
To see details of my list please click on the image below, or visit this page.

,
- Migraine: stigma and misunderstanding
Although medical topics are more openly discussed nowadays, some diagnoses seem more socially acceptable than others. People are quite happy to talk loudly in cafes about their heart attacks and hip replacements, but not about conditions likely to evoke fear, disgust, disapproval – or disbelief, in cases of “invisible” illnesses that are not clearly defined or understood.
When I have been injured in falls caused by my own recklessness while playing with exuberant dogs or running on slippery rocks, other people have always been helpful and sympathetic. Such a contrast to the negative reactions I have sometimes received in relation to migraine, and I know that my experience is not unique. People who have never had an attack themselves may assume migraine to be “just a headache”, or “all in the mind”, a trivial indisposition being exaggerated to gain sympathy or avoid unwanted obligations, and brought on through the sufferer’s own fault.
Research over recent years has identified some of the genes which predispose to migraine, and some of the physiological changes that take place during attacks, and migraine is now classed as a neurological disease. But its validity is not always recognised because it is a complex condition that can present in a wide variety of ways and follow a variable course, and there is no diagnostic test. Other conditions which have a consistent symptom pattern accompanied by specific abnormalities of biochemistry, pathology or Xray, are more likely to be taken seriously.
Someone in the throes of a severe attack, prostrated by pain and vomiting, is clearly very unwell. But in between attacks they may look and feel quite healthy, so that observers cannot believe there is anything wrong with them, and do not understand why they may be trying to control their condition by lifestyle measures. For example, while it would be accepted that someone with diabetes needs to follow certain rules about diet, a migraineur wanting to avoid “trigger foods” when out for a meal risks being considered rude and fussy.
Some of the stigma around migraine may be blamed on lingering sexist attitudes within the medical profession. Historically, certain doctors labelled their female migraine patients as neurotic, hypochondriacal and frigid, while describing their male ones as responsible, ambitious high achievers. Psychoanalysts have claimed, usually without any evidence, that the attacks represent sexual conflicts or the outburst of suppressed emotions such as anger or disgust. Such theories are less fashionable now that the biological basis of migraine is established, but have not entirely disappeared.
Lastly, though I am reluctant to admit it, I believe that migraineurs themselves can play a part in perpetuating stigma. My husband has told me that my personality appears to change during attacks, and not in a good way. If this is true for me and others, maybe we unknowingly give off “vibes” that confuse and alienate people. A projection of the guilt or shame we ourselves may be feeling at these times? If we were better able to retain our self-respect, and not try to hide the attacks nor apologise for them, we might get fewer hurtful responses.
Migraine and Me: A Doctor’s Experience of Understanding and Coping with Migraine by Jennifer Barraclough is available in e-book or print versions from Amazon and other online retailers.
- Too many photos
Since buying my first iPhone I have taken thousands of photos, which have been stored rather haphazardly in various locations on my computer, some identified only by their numbers. I recently resolved to declutter and reorganise my digital files, prior to updating my devices. Labelling all the photos and allocating them to folders has proved a massive task, made harder because of my somewhat obsessional nature. How to classify them? Some belong in more than one category – animals, husband, family, friends, holidays, me with different hairstyles. Which to keep? I don’t like deleting any, apart from a few duplicates and photos of people I no longer recognise.
The project – still not quite finished – has sometimes felt overwhelming. For a while I was rushing to get it done, and wishing I hadn’t started it at all. But it seemed too late to give up, so I resolved to take a more thoughtful approach and appreciate all the images for the happy or sad memories they evoked.
Doing this has been a poignant reminder of the transience of life. Many of the people and animals in the photos have now died. The appearance of myself and my husband has changed over the years, and not for the better. I may never want to look back at these files again myself, and I have no close family so nobody else will want to keep them after my death. Anyway, they might all have been wiped out by some technical disaster by then. I was reminded of the Tibetan Buddhist monks who create beautiful mandalas made of coloured sands, and then deliberately destroy them.
Only read on if you like cats. I usually include some photos in my posts, but couldn’t decide which to choose from among so many, so I decided just to feature the cats who have lived with us since we moved to New Zealand. Excluding all the foster kittens, there have been seven long term residents, two of whom – Magic and Leo – are still alive. It was quick and easy to find their photos, which made me think that the project has been worthwhile after all.

Cinderella 
Floella (daughter of Cinderella) 
Felix 
Daisy 
Homer 
Magic 
Leo - Preventing migraines – beyond medication

Feverfew, Tanacetum Parthenium This is not an “anti-drug” post – I fully accept that prescribed medication is the mainstay of migraine prevention. Certain beta-blockers, antidepressants and anticonvulsants are long established for reducing the frequency and severity of attacks, and the newer CGRP inhibitors have even better results. But none of these drugs work for everyone, and all of them can have unwanted side effects. I took propranolol for many years with some benefit, but then its effect seemed to wear off. I then decided to look more closely at what lifestyle factors triggered my attacks, and to explore some complementary therapies that seemed more “natural” and gave me more choice and control over managing my health. Many of the non-drug options for migraine prevention are supported by evidence from clinical trials as well as by anecdotal reports, but the orthodox medical approach tends to focus on drug treatments alone. My new book Migraine and Me: A Doctor’s Experience of Understanding and Coping with Migraine aims to give a more holistic overview. Here is a brief summary of some of the preventive methods it describes. They do not offer a cure for migraine but, whether used alongside drugs or instead of them, they can help. Most of them are relevant to other chronic medical conditions too.
Being instructed to eat better food, get more sleep, take more exercise, stop smoking, drink less, and reduce stress can be irritating – but these deceptively simple “healthy living” guidelines can make a real difference. There are special considerations for migraineurs such as not going too long between meals, and identifying triggers in the diet and environment.
Dietary supplements which have been found effective include magnesium, B vitamins and Coenzyme Q. The herb feverfew, illustrated, is available in capsule form but the most natural way to take it is by chewing its leaves, as described in one of the case histories in my book.
Relaxation techniques can help by activating the parasympathetic “rest and digest” branch of the nervous system, as opposed to the sympathetic “fight or flight” branch which tends to be overactive in migraineurs. Relaxation is a component of many other therapies such as biofeedback and massage.
Psychological therapies may be regarded with suspicion because they are thought to imply that migraine is “all in the mind” rather than being a neurological disease with a genetic basis. I am certainly wary of psychoanalytical theories that cite repressed anger or sexual conflicts as being the cause. But more practical approaches such as cognitive behavioural therapy (CBT) can alleviate the mental distress and social difficulties that make it harder to cope with attacks and may well be exacerbating them.
Creative activity through art, music or writing is a way of processing emotions around migraine. If the results are made public, they can contribute to understanding of the condition. Some works by historical figures such as Richard Wagner and Vincent van Gogh are thought to have been inspired by the migraine experience.
These and other approaches are covered in more detail in Migraine and Me: A Doctor’s Experience of Understanding and Coping with Migraine, available in both print and e-book versions from your local Amazon site and other online retailers. Please forward this post to anyone in your circle who may be interested.
- When is it time to stop?
Watching Joe Biden’s determination to cling on to power despite his obvious physical and mental decline has made me think again about a question that keeps arising as I get older: Is it better to stop doing things while the going is good, or to carry on till it is clear you are not coping?
I am a few years younger than Biden. I feel fit and well, in fact better than before since my sleep pattern has improved and I have grown out of the migraines that plagued my earlier life. And yet, looking back over the last few years I realise what a lot of my former activities I have given up. This has sometimes been because of external factors outside my control, such as family illnesses and transport difficulties and lockdown effects, but also reflects the gradual loss of energy and confidence that comes with aging.
Not all the changes are bad. My life is quieter, and more locally based. I still enjoy driving but no longer fancy long trips, which must reduce my environmental footprint. I have resigned from my previous choir over in Auckland city, but joined another which is nearer and requires less time commitment. I don’t do sessions at the animal rescue centre any more, but help to look after two dogs as well as my own two cats. I closed my Bach flower client practice some time ago, but still make up remedies for friends. Instead of the film society in the city, I go to the local cinema or watch DVDs at home. I have joined a book group, dance and TRX exercise classes in the village where I live, and made a few new friends there. I still love writing and would hate to give that up, yet I don’t write as fluently as I used to, nor do I have so many new ideas. I don’t want to be like well-known authors such as Agatha Christie and PD James, whose later novels were so inferior to their early ones. Perhaps my latest book Migraine and Me will be my last.
There may come a time when someone wanting to continue as an active and productive member of society becomes a nuisance, an embarrassment or worse. But this is not inevitable. Older people can have much to contribute due to their long experience of life, and it is a mistake to underestimate them on grounds of age. The English environmentalist and chimpanzee expert Jane Goodall recently undertook a lecture tour around the world at the age of 90, and I’m told that her presentation in Auckland was inspiring.

Jane Goodall with a chimpanzee - Last Night of the Proms – New Zealand style

Along with a big crowd of other British expats wearing red white and blue, I attended a joyful and nostalgic version of the Last Night of the Proms performed with orchestra and choir in the Bruce Mason theatre on Auckland’s North Shore.
The programme began with God Save the King and finished with Rule Britannia, Land of Hope and Glory and Jerusalem, with many other traditional items in between. New Zealand content included the national anthem, a Maori song called A Te Tarakihi, and a film of the Spitfire flying at the Warbirds air show. The soprano soloist wore a series of splendid gowns, one resembling a giant Union Jack. I used to think I hated bagpipes, but the wonderful performance of Highland Cathedral by a pipe band was a highlight of the show.
Towards the end, the hall filled with balloons and streamers as the wildly enthusiastic audience sang along and waved our flags. We all had a good time, and perhaps some of us were left wondering whether the UK or NZ feels more like home.

- Migraine and Me – the ebook

I’m pleased to announce that Migraine and Me: A doctor’s experience of understanding and coping with migraine is now available as an ebook from Amazon Kindle and various other online retailers as listed on this link, with a print version planned to follow soon.
My migraines began in my teenage years and continued until later life. In this short book I’ve combined personal stories from myself and other contributors with information from published research. Writing both as a (retired) doctor and as a (recovered) migraine patient, I’ve aimed to balance the medical aspects with the psychological, social and even spiritual ones. The book describes how lifestyle measures and complementary therapies, as well as prescribed drugs, can help to prevent attacks. It covers some sensitive topics such as the concept of a ‘migraine personality’ and the reasons for stigma, and ends on a positive note with sections about creativity and ‘silver linings’.
To quote from the blurb: “Migraine and Me offers empathy, practical insights, and hope for anyone affected by this complex neurological condition, once described in a drug advertisement as hell on earth.”
If there is anyone in your circle who is affected by migraine and might be interested, please share this post with them. Here again is the link to the book.
- eBooks old and new
My new ebook Migraine and Me is nearly finished but I’ve left the final draft aside for a while, so I can check it through with fresh eyes before publication.
Meanwhile I’ve been continuing my project of “Going wide with D2D”. The aims are to bring some of my earlier books to a wider readership, and to update my basic skills in formatting text and using self-publishing technology. So Wellbeing for Writers and Beautiful Vibrations are now available not only from Amazon Kindle (kdp) as before, but also from many other ebook retailers as shown on this link http://books2read.com/jenniferbarraclough.

“A short practical guide about how to enjoy the journey to becoming a (self)published author, and how to cope with challenges such as lack of time for writing, lack of inspiration, negative criticism, and aversion to marketing. Jennifer’s experience as an author of both fiction and non-fiction books, combined with many years of working with clients in various therapeutic settings, has given her a wide personal understanding of the psychology of writing. This little book includes many practical tips for making the process run smoothly, and enhancing mental and physical wellbeing.”

“Anxiety, sadness, anger and loss of hope are common responses to serious or chronic illness. Symptoms of the condition itself, side-effects of treatment, concerns about diagnosis and prognosis, restriction of activity, and changes in relationships take their toll on both body and mind. Ideally, negative feelings will soon be replaced by a more positive adjustment, but sometimes they are severe or prolonged. Bach flowers are not a cure for physical disease but help to relieve the emotional distress often associated with it. Dr Edward Bach described them as having ‘beautiful vibrations’ capable of promoting positive mental states such as hope, courage and calm. This practical guide, illustrated by case histories and flower photos, explains how to select and use the remedies as part of a holistic approach to healing. Despite all its unpleasant aspects, the experience of illness can have a silver lining and the flower remedies help to bring this out.”
- My husband’s heart Part 4: TAVI

In 2015 my husband Brian had major cardiac surgery. I wrote some posts describing his operation and gradual recovery on this blog – here are the links to Part 1, Part 2 and Part 3. Now it’s time for another episode. Writing about these experiences is my way of processing them, and maybe reading about them will be helpful for other patients and their partners who are going through something similar.
The operation was successful, and Brian remained fit and active both physically and mentally for the next eight years. Then he became slightly less well, with a more irregular heartbeat, and more shortness of breath when climbing up the 68 steps on the hill behind our house. These changes happened slowly and neither of us took too much notice – after all, it would seem normal to be slowing down at the age of 90. But after seeing the results of Brian’s routine followup echocardiogram, his cardiologist was concerned and arranged a series of further investigations.
These included a Transoesophageal Echocardiogram, CT Coronary Angiography, and Coronary Angiogram. Performed at weekly or fortnightly intervals, with blood tests in between to check Brian’s renal function, each of these tests involved spending a long morning at our local North Shore Hospital. They were not without risk, because they required sedation and/or arterial injection of contrast media, but Brian tolerated them well. He was understandably anxious during this period and I gave him a course of Bach flower remedies, Mimulus and White Chestnut, which seemed to help. When all the tests were complete we saw the cardiologist again. He said that the porcine aortic valve inserted in 2015 was broken and that Brian needed another operation “soon” – otherwise his prognosis would be very poor.
Brian said that he didn’t feel ill, so was rather reluctant to have another operation at his age, even though it would be a far less invasive procedure than the open heart surgery he had before. But he did agree, and on the following Monday I got a call from Auckland City Hospital asking us to come straight in that afternoon. Brian was given a single room, and hooked up to an ECG monitor. I tried to concentrate on reading while he had various tests, was visited by the anaesthetist and cardiologist, and was shaved all over in preparation for his TAVI at 7.30 a.m. next day. I went home in the evening and fed the cats.
TAVI stands for Transcatheter Aortic Valve Implantation. The procedure, which takes about two hours, is carried out under light anaesthesia. It involves making an incision in the groin to access the femoral artery, through which the new valve (formed from either porcine or bovine tissue) is delivered to the heart on the end of a catheter. Another incision is made in the radial artery, near the wrist, for the injection of contrast media to allow the procedure to be monitored by x-ray. There is a large team of clinicians involved: two interventional cardiologists, a specialist nurse, other nurses, cardiac physiologists, and radiographers.
It seemed pointless for me to go back to the hospital until Brian was out of the operating theatre, so I stayed at home and occupied myself by changing the bedlinen. In the middle of the morning a doctor rang to tell me that the operation had been completed successfully. I had not realised quite how stressed I was feeling until, on hearing this news, I burst into tears. When I returned to his room about noon I found Brian conscious and lucid though looking rather strange, with most of his body covered in a red dye, and wound dressings on his arms and legs.
Having had another echocardiogram to check that his new valve was working well, Brian was discharged the evening after his operation. A few days later he was feeling reasonably well, still needing to rest much of the time but able to go out for short walks. Full recovery is likely to take a month or two. It is wonderful to see what modern medical technology can achieve, and hopefully Brian’s TAVI will be followed by another long period of good health.
Update: I was going to publish this post last week but then Brian had a serious setback due to bleeding from the bowel. Apparently this can happen after a TAVI for various reasons. He required emergency admission to hospital and was very unwell for several days, but improved after a series of blood transfusions, and is now happy to be back home. He needs to rebuild his strength, and will be having further outpatient investigations to see whether there is a correctable cause for the bleeding.
- Bach flower remedies for the management of migraine

The Bach flower remedies are not intended to treat migraine or any other medical disorder directly, but to correct any imbalances of mood or personality which may be associated, whether as cause or effect. They are among the many “complementary” modalities which can aid in the management of this complex condition.
The system was developed in England by Dr Edward Bach almost a hundred years ago. Through intuition, he identified a series of wild flowers corresponding to the emotional states of people and animals. This may sound unscientific and bizarre, but the therapy continues to be widely used around the world, and a number of clinical trials have testified to its effectiveness: I am one of the practitioners contributing to a new database of published studies which can be found at https://www.cambridge-bach.co.uk/bach-science-studies-database/ . The remedies, prepared in liquid form and taken by mouth, carry the energetic signature of the source plant. They are safe and free from side effects, having no chemical content apart from the low concentration of brandy used as preservative. An individualised mixture, containing up to six of the 38 remedies, is chosen for each client.
Because the therapy is prescribed for the person not the disease, there is no standard formula for migraine. Theoretical examples of flowers to address the emotional burden of the condition include Mimulus for fear of more attacks, Elm for feeling overwhelmed by responsibilities, Gentian for being discouraged about the lack of improvement, Red Chestnut for worries about how the attacks are affecting others. Treatment needs to be continued for several weeks to have a lasting effect but can be short-term for acute situations and Rescue Remedy, a combination of five flowers available as spray, can have a calming effect in the early stages of a migraine attack.
Whether or not a “typical migraine personality” exists, any long-term traits of personality which are making life more stressful could be contributing to attacks. Philip Chancellor’s book Illustrated Handbook of the Bach Flower Remedies, published in 1971, reads as somewhat old-fashioned but contains many interesting case histories from the records of Dr Bach’s clinic in the Oxfordshire village of Brightwell-cum-Sotwell. It describes five women with migraine, all of whom improved on remedies chosen according to their personality type. These included Chestnut Bud for being slow to learn from experience and repeating the same mistakes in life; Oak for working to the point of exhaustion due to a strong sense of duty; Scleranthus for an inability to make decisions; Vervain for being unable to relax due to over-enthusiasm; Wild Rose and Centaury for a woman passively resigned to being dominated by her husband and having no life of her own.
Two of my own books are relevant to this topic. Beautiful Vibrations: Living through medical illness with Bach flower remedies and Migraine and Me: A doctor’s experience of understanding and coping with migraine. Both are available in print or e-book formats through major online retailers.
- Migraine’s silver linings
This is another draft extract from the book based on my personal experience of migraine which I am currently writing and hope to publish in the next few months. I would like to include some short contributions from other people too, so if you have anything you would like to share in relation to this post or any other aspect of migraine, please leave a comment below or write to me through the contact page of my website jenniferbarraclough.com.
I am rather sceptical about claims that illness is a “gift” or a “lesson from the universe”. I think my life would have been much happier if I hadn’t had migraine. But no experience is entirely bad, so this post is my attempt to find some positive things to set against the hardships.
Having migraine provides a strong incentive to lead a “healthy lifestyle” – a nutritious diet, enough exercise, enough sleep, managing stress. For migraineurs it is especially important not to go too long without eating, not to over-indulge in food and drink, to avoid known triggers, and to maintain a reasonably regular daily routine. The self-discipline needed to stick to these guidelines can be tedious. But it will hopefully be rewarded not only by having fewer and less severe migraine attacks, but also by a reduced risk of many other medical disorders and of accidents, and an improvement in general wellbeing.
Activities which disrupt the daily routine too much are quite likely to bring on a migraine, spoiling the occasion for oneself and others, so it can be prudent to avoid them. Sometimes this is disappointing, for example when I decided not to accompany my husband on a trip to a beautiful island because it would involve an early morning start, a choppy sea voyage, and a strenuous walk before lunch. On the other hand migraine provides a good reason to be selective about how to use time and energy, rather than waste them on things which are neither enjoyable nor worthwhile. The temptation to cite migraine as an excuse to shirk unwelcome obligations should of course be resisted ….
While being less active in the outside world, there is more time to spend quietly at home, giving opportunities for rest and relaxation and creative activities. As discussed in another chapter of my forthcoming book, the migraine experience can inspire creativity, especially for painting but also in music, fiction and poetry. I haven’t made much use of my own migraine experience in my writing, except once in a short novel called Fatal Feverfew, which would seem quaintly old-fashioned today.
Over the years, outside of my career in orthodox medicine I’ve explored many systems of personal development, psychotherapy, natural healing, religion and philosophy. This has been mainly out of general interest but partly motivated, consciously or not, by the futile hope of finding “the answer” to my migraines. I’m not sure how much anything helped with the attacks themselves, but I have learned to cope with them better and to become more skilled in dealing with other people’s reactions. Hopefully all these studies have also made me a better-informed and more tolerant person.
As a final comment it is reassuring to know that, except in very rare cases of stroke during an attack, migraine does not cause permanent brain damage or cognitive impairment. And although migraine carries a raised risk of cardiovascular disease, the risk of developing diabetes or cancer is reduced, and the overall death rate is not increased. Most migraineurs therefore have a normal life expectancy, and maybe the best thing that can be said about migraine is that after the age of 70 it often goes away.
If you have found any positive aspects in your own experience of migraine I would be interested to know about them.
- Stress, migraine and me
This is another draft extract from a book based on my personal experience of migraine which I am currently writing and hope to publish next year. I would like to include some short contributions from other people too, so if you have anything you would like to share about this or any other aspect of migraine, please leave a comment below or write to me through the contact page of my website jenniferbarraclough.com.
Stress is known to contribute to many medical disorders, presumably because of the impact of hormones such as adrenaline and cortisol, generated through the sympathetic nervous system, upon the body and brain. Many migraineurs cite stress as their top trigger factor, while others vehemently deny that stress has anything to do with it at all. Some of my own attacks have clearly been induced by stress, whereas others have apparently come out of the blue. Many people talk of stress without really thinking what they mean, and it is too easy to say of migraine or any other condition “It’s due to stress” or worse “It’s just due to stress”, when this may not be the case at all and is certainly not the whole story.
Feelings of stress are usually blamed on outside circumstances, the negative events and ongoing difficulties which are an inevitable part of life. But it is individual responses which determine how stressful these experiences are perceived to be. Responses depend both on mental attitudes and physical constitution. There is evidence that the sympathetic nervous system tends to be overactive in migraineurs even between attacks, causing them to live in a state of chronic low-grade physiological stress, perhaps without knowing it. This would explain why therapies which promote relaxation, such as biofeedback, are effective for migraine prevention.
One common source of stress is an accumulation of the hassles and demands of everyday life in the modern world – juggling work, household and family responsibilities, financial strain, discord in relationships, transport delays, a deluge of emails and media posts. Pressure can intensify at times which are supposed to be enjoyable, such as holidays or Christmas, when organising the preparations is combined with changes to routine and possibly physical stress from lack of sleep, unfamiliar foods or missed meals, and excessive exertion.
Even when there is no external cause, people can generate stress for themselves by setting unrealistically tight deadlines or high standards, mulling over regrets about the past or anxieties about the future.
Migraine itself is a potent source of stress, and vicious circles can develop, as in the case of someone who is worn out after a busy period at work, gets a severe migraine and has to take a few days off. There is nobody else to cover for them, so on returning they find a backlog of tasks has built up so that the workload intensifies, and leads to another attack. After this scenario has been repeated a few times they either lose their job because of being unreliable, or feel compelled to resign, and then experience the stress of unemployment and financial hardship.
The relationship between stress and migraine is not straightforward. It is recognised that some migraineurs manage to cope with intense pressure during the week, but get an attack at the weekend when in theory they have time to relax. Not all stress is bad. In the days when I was prone to severe migraines, I found that working very hard on a project that was important to me did not bring on an attack. Situations in which I felt frustrated and not in control, for example having to attend long meetings of little interest or wait hours in airports for delayed flights, often did.
I may be wrong but I have the impression that major crises, stressful though they are, do not necessarily trigger migraines and might even protect against them. A woman once told me that her severe and frequent attacks had stopped for several months following the sudden death of her child. I experienced something similar a few years ago when my husband was critically ill at the same time as my mother was dying. Although I became unwell myself with other mental and physical symptoms during this period, I did not get any migraines. I have never seen this phenomenon described in the literature and would be interested to know if others have experienced it.
- Going wide with D2D
In the world of indie publishing, “going wide” means listing books on several platforms rather than just one. Until now my self-published ebooks have only been available through Amazon KDP (Kindle Direct Publishing), though the print versions were already distributed more widely. Amazon has led the way in enabling writers to publish their work at minimal cost and I had been quite happy dealing with them over the years. But many complaints about their customer service can be found online, and I recently had a frustrating experience myself.
I was unable to access my KDP account because the one-time passwords (OTPs) were no longer coming through to my iPhone. I wasted hours on repeated failed attempts, online chats and calls to America. The customer service agents all tried to be helpful and suggested various solutions, which included sending copies of my passport and driving licence to Amazon. Nothing worked. I eventually discovered from another author on a local Facebook group that the problem was nothing to do with me personally, but affected all New Zealand phone numbers, and the remedy was to use an authentication app instead of an OTP.
This saga prompted me to look at other options, and so far I have republished two of my ebooks through the distribution platform Draft2Digital (D2D). These books are still available on Kindle, though no longer in the exclusive “Select” program, but are now also listed by many other retailers worldwide. I found D2D easy to use, because authors just need to upload their text, and D2D’s computer will deal with formatting and add details such as the title page and table of contents if required. I sent a couple of queries to the help desk and received helpful and intelligent replies.
The next challenge is to sell more books, and this is the difficult part. I love the process of writing them, and also enjoy learning the basics of how to format texts and upload them to the internet. But I thoroughly dislike marketing and seldom do any, other than via occasional posts on this blog, and therefore get very few sales. That doesn’t matter from a financial viewpoint because I don’t depend on authorship as a source of income. But it is nice to earn a little money in return for all the work I’ve put in, and more importantly to know that some people read and hopefully enjoy what I write.
So if you haven’t seen them already, please have a look at my two most recent novels which are both gentle mystery stories involving family relationships and domestic crimes. You Yet Shall Die is set in rural England with a timeline ranging from the 1940s to the 2000s. Cardamine is set in New Zealand just before the Covid pandemic. The ebook versions are available from many different retailers as well as Amazon; have a look through this link.


- Don’t pat strange dogs – Updated
While out and about I always say hello to the dogs I meet, and most of them want to be friendly. I have patted hundreds of them over the years, and never been bitten – until last week. I was walking past a cafe where a medium sized black dog was sitting with his family at an outside table. Our eyes met. I began to approach him, assuming he wanted a pat, but he suddenly lunged forward and sank his teeth into my hand. It was a deep bite and very painful. I went into shock and almost fainted. The dog’s devastated owner and the cafe staff were very helpful, bringing me water and putting iodine and a plaster on the wound. After a while I felt well enough to continue on my way.
The pain continued all day, and by next morning my whole hand was red and swollen. My husband came with me to the emergency department of our local hospital. I was seen by a specialist nurse who gave me a tetanus booster and some blood tests, arranged for a hand X-Ray and admission to the orthopaedic ward.
The ward was full, so I spent the first day receiving my intravenous antibiotics in the corridor of a crowded and noisy medical assessment unit. I was transferred to a spare bed in a gynaecology assessment unit overnight, and finally reached the orthopaedic ward before lunchtime next day. This was not ideal but the important thing was having been promptly started on treatment, without which I realise I could have lost an arm or even died.
Being in hospital was a new experience for me and not nearly so bad as I expected. All the staff I encountered were skilled, efficient and kind. It was interesting to chat to other patients, and good to receive visits and messages from family and friends. I felt surprisingly well during my stay but it was a while before the cellulitis began to resolve. I was scheduled for surgical drainage on the third day, but by then the operation was judged to be unnecessary and I was discharged home to continue on oral medication for another week.
Dogs usually bite because they feel threatened, and it is those who have been abused as puppies who are more likely to become aggressive in later life. The owner has kept in touch and I hope to meet him again to find out something about the culprit’s background and character, and try to understand why I provoked him. I will be more cautious in future about patting strange dogs.
Update March 2024
Three months after the events described above, I arranged to have coffee – in a different café – with the family of the dog that bit me. As I suspected, Baxter (not his real name) had been cruelly treated in early life, during that vital period from about 8-16 weeks which can make or mar a dog’s temperament. He was born overseas in a puppy mill, transported long distances, and surrendered to a rescue centre before being adopted by his present owners. Even after some years in a loving forever home, he still has some behaviour problems, and is now having professional therapy. When I saw him at a distance he regarded me suspiciously. I have let go of any fantasies about making friends with Baxter, but seeing him and his family again gave me a worthwhile sense of “closure”, and I wish them well on the long journey of rehabilitation for a dog who has been so damaged by early abuse. By the way my hand wounds have healed well, leaving just a tiny scar to remind me of what happened.
- Food, drink, migraine and me

Photo by Chelsea Pridham on Unsplash This is a draft extract from a book, based on my personal experience of migraine, which I am currently writing and hope to publish next year. I would like to include some short contributions from other people too, so if you have anything you would like to share about this or any other aspect of migraine, please leave a comment below or write to me through the contact page of my website jenniferbarraclough.com.
People who are vulnerable to migraine often report that dietary factors – foods, drinks, and meal patterns – can trigger their attacks, and this is certainly true in my case. Eating cheese is the worst thing for me. It took many years to recognise this, which now seems strange, but because it was something I used to eat almost every day when I was younger I didn’t notice a connection. Also, this was years before it was possible to look up health information on the internet, and we were not taught much in medical school about relationships between diet and disease. Cheese, especially strong aged ones, is implicated for other migraineurs too and this is believed to be because it contains high levels of a biogenic amine called tyramine. This substance gets metabolised in the gut by an enzyme called monoamine oxidase, but people who only have low levels of this enzyme cannot process it fast enough, so that it builds up in the body and can cause not only migraine attacks but also increases in blood pressure and symptoms such as nausea, sweating and anxiety. Other high tyramine foods which are sometimes implicated in migraine include chocolate, processed meats such as bacon and salami, smoked fish, raw onions, fermented or pickled vegetables, broad and fava beans, oranges and other citrus fruits, ripe bananas, pineapples and avocados. None of these disagree with me like cheese does, so I suspect that the combination of chemicals besides tyramine found in different items of food is involved in individual sensitivities. While some migraineurs benefit from a low tyramine diet, others have reported benefit from gluten-free, dairy-free or ketogenic diets, or from giving up all forms of sugar.
While some foods may be best avoided, the good news is that others – those containing high levels of omega-3 fatty acids – have been found to reduce the frequency and severity of attacks. They include oily oily fish, dark leafy greens, chia seeds, flaxseed, tofu, walnuts, and eggs.
Alcoholic drinks are often blamed for precipitating migraine attacks. This may not be due so much to the alcohol itself, as to the fact that they contain various other chemicals, again including tyramine. I love wine, so am glad to say that white or rose in moderation is not a problem for me, in fact it is probably helpful because of its relaxing effect. Red wine is more risky, and is notorious for provoking headaches even in people without migraine, probably because of its quercetin content. I seldom drink more than one glass of anything nowadays, having found in the past that just a slight excess can be followed by a whole day of feeling very ill with a ghastly mixture of migraine and hangover symptoms. When cheese and wine parties were fashionable they often proved a disaster for me.
Coffee, and other caffeinated drinks, are migraine triggers for some people. I am fine with one double shot flat white or Americano mid-morning, but not more. Sudden withdrawal of caffeine can also lead to an attack, so it is best to keep a fairly constant intake. A few years ago I spent a week at a health resort where coffee was forbidden. I had cut down on it the week before but still had a nasty headache for the first three days, though this did not develop into a full-blown migraine. Paradoxically, caffeine is present in some over-the-counter medicines for migraine, and black coffee has been found helpful during attacks as a treatment for people who do not usually drink coffee at all.
The timing and size of meals is important, as well as the type of food and drink they contain. Going too long without food or water can precipitate a migraine attack, but so can eating too much at one time, so it is important to maintain a reasonably regular meal schedule and to avoid dehydration.
Food triggers may be hard to identify because there can be a delay of hours or even days before their effects develop. If someone gets a migraine soon after eating a certain type of food they may develop a fear of that item and avoid it in future, although the attack may actually have been caused by something else. There may be a psychological element involved – for example if I have given in to the temptation of eating a piece of cheese, I usually worry about it afterwards and my anxiety may increase the likelihood of an attack.
Avoiding alcohol, caffeine and all suspected food triggers requires a lot of will power, is awkward in social situations, and makes for a somewhat joyless existence for those who enjoy eating and drinking. Some of the “migraine diets” to be found on the internet appear impossibly restrictive and might even cause nutritional deficiencies in the long term. Dietary triggers are not the same as allergies in which eating even a tiny amount of a certain food, peanuts for example, is quickly followed by a severe reaction or even death. Many migraineurs can get away with eating their trigger foods in small amounts now and then provided they are not exposed to other risk factors at the same time.
- Researching Bach flower remedies

My home remedy box Since training as a Bach Foundation practitioner twenty years ago I have carried out several hundred client consultations, and though now officially retired I still sometimes make up remedies for friends. Presenting problems may involve emotional distress linked to difficult life circumstances or relationships, medical illness, bereavement, and/or longstanding personality traits. The therapy involves selecting a mixture, containing between one and six of the 38 flower essences, for each individual case. My experience has convinced me that if the mixture has been chosen and taken correctly it usually has beneficial effects. But is this due to a specific action of the remedies or to general factors such as expressing feelings during the interview, taking part in selecting the prescription, and positive expectations due to a mystique around the energy of flowers?
There are descriptive reports of Bach flowers being used with benefit in psychiatric and medical settings, general practices and hospices. Primarily given to balance the emotions, they can also help to alleviate physical symptoms in which anxiety is playing a part. However many orthodox clinicians – if they have heard of the remedies at all – dismiss them as rubbish because conventional science cannot explain how they could work.
It should be possible to evaluate Bach flower therapy with clinical trials in which subjects are randomised either to a treatment group receiving a genuine remedy mixture, or to a placebo group receiving mineral water. A number of such trials have been reported from around the world, outcomes being assessed with psychological and/or physiological measurement scales. I have joined a small group of practitioners who are reviewing published papers, and posting summaries and comments to a database which can be found at https://www.cambridge-bach.co.uk/bfr-clinical-trials/. Several of the studies reviewed so far indicate that Bach flowers have positive effects: for example reducing anxiety in children attending a dental clinic in India, reducing stress and insomnia for staff of a hospital in Spain, supporting the process of labour for women in a maternity unit in Brazil.
Some of the studies have limitations, for example:
- Giving the same combination of flowers to everyone in the treatment group. This may appear “scientific” and obviously saves time, but is not a fair test of the therapy because a standard formula would not be expected to work so well as an individual mixture chosen through interview with a trained practitioner.
- Lack of a proper randomised double blind placebo controlled design. It is essential that neither the subjects in the study nor the personnel carrying out the interviews know who is in the treatment group having real remedies, as opposed to the control group having mineral water.
- Presenting the results in statistical tables too complex for most people to understand – hardly in keeping with Dr Bach’s core value of Simplicity! It would be useful to include some description of subjective experience as well as the numerical data.
We will gradually be adding more studies to the database, and even if their methodology is not always perfect, taken together they may provide enough evidence to convince sceptics that Bach flowers do work. Being non-toxic and low-cost, these remedies could be valuable as a complementary therapy in almost any setting.
- Bottle babies: feline neonatal care
I have fostered many homeless kittens over the years, but none less than 10 weeks old. I recently attended a workshop at my local animal rescue centre to learn about fostering neonates. These have usually been brought in by members of the public who have found an abandoned litter without a mother cat. Caring for these orphaned newborns is a full-time job requiring great dedication, as they need attention every 2 hours both day and night if they are to survive. After arrival at the centre they are allocated to a foster parent who can pick them up as soon as possible and take them home along with all the necessary equipment: carry cage, towels and bedding, microwavable heat pad, formula feed, bottle and teats, digital scale and bowl for weighing, syringes and toileting cloths.
The care routine, as demonstrated on a stuffed toy at the workshop, involves preparation and warming of formula food, hand washing, toileting, weighing, bottle feeding, toileting again, cleaning, burping, changing the bedding, cleaning the bottle, hand washing again, and recording notes to send in to the centre. The process is then repeated for the next kitten. It is best for each foster home to have more than one, so they can learn to socialise and play with each other.
They will spend the first 3 weeks in their cage, then at 3-5 weeks move into a larger crate, and then when they have learned to feed themselves and use a litter tray they have access to a small secure room but are not allowed outside. When they can eat solid food and have reached about 1 kg in weight, usually at 8-10 weeks of age, they return to the centre to be desexed, microchipped and vaccinated. Some will need a further few weeks of fostering, for example if they are still on medical treatment. They are then ready to go to their forever homes. Kittens at this stage are very appealing and are usually adopted within a few days of becoming available. Sometimes the foster parents can’t bear to part with them, as was the case with Magic and Leo (pictured) whom we decided to keep after fostering them 8 or 9 years ago.

Leo
Things do not always go smoothly. Small kittens from deprived backgrounds are vulnerable to infections such as cat flu, ringworm and Giardia. For this reason they need to be checked daily for symptoms such as lethargy, loss of appetite, diarrhoea, vomiting, sneezing, discharge from eyes or nose, scratching or hair loss. They also need to return to the centre once a week to be examined by a vet. Not all of them will survive, sometimes due to a condition called the fading kitten syndrome, which can develop for many reasons though often the cause is unknown. One friend of mine has questioned the wisdom of putting so much effort into saving their lives, when there are so many unwanted cats in New Zealand. But it would seem very hard hearted to let them die. A better solution to overpopulation is desexing, which is now being stepped up again having been suspended during the Covid pandemic.
Maybe reading this post will encourage others to consider neonatal fostering, After reflecting on the content of the workshop, I don’t think I have enough physical or mental stamina for the night work involved in looking after “bottle babies”, but I look forward to taking in some slightly older kittens again this summer.
- Learning the piano – with cats

Daisy was a major distraction I am resuming my efforts to learn the piano. I doubt I will ever achieve my ideal of playing Bach with fluency, but it would be nice to be good enough to play simple pieces for my own pleasure. Also, having reached an age when an alarming number of my friends are developing dementia, I hope it will help to preserve my brain power. Studies have shown that playing the piano improves memory, mental speed, concentration, and eye-hand coordination, as well as decreasing anxiety and boosting happiness and self-esteem.
As a child I had a few lessons which I didn’t enjoy, though I was glad of them when I started playing again after a gap of several decades and found I still remembered some basics which might have been hard to learn later on. I know it is important to have a teacher to encourage regular practice and progress along the right lines, but it can be hard to find a good one. I have had a couple who were mediocre, and one who verged on the sadistic – I imagine it must be frustrating for skilled musicians to have to earn a living by giving lessons to slow learners like myself. My most recent teacher was excellent but he is no longer available and will be hard to replace.
I have some excuses for failing to practise as much as I should. A major setback was breaking my wrist and being unable to play at all for almost a year. Movement of my right hand is permanently restricted, and it becomes painful if I use it for too long. The other main impediment is the presence of cats. When Daisy (pictured) was alive, she delighted in jumping onto the keyboard and marching up and down, with a preference for the bass. I sometimes wish I could have trained her to play proper duets with me, after the fashion of Nora the Piano Cat whose YouTube videos have brought her worldwide fame. Nora is a grey tabby, adopted as a kitten from a rescue centre and now almost 18 years old – a feline example of the health benefits of playing the piano? One of our present cats, Leo, distracts me by scratching rhythmically on some nearby piece of furniture whenever I start to play. Our other cat, Magic, has no interest in music at all.
- “Three Novellas” ebook free this week
The ebook version of my Three Novellas is free on Amazon this week. It includes three gentle rather old-fashioned stories which, as it says in the blurb, “include elements of romance, medical mystery and the paranormal, reflect the author’s experience of practising as both orthodox doctor and alternative healer, and her leisure interests including animals and music”. I wrote them in the early 2000s, inspired by my experience of living between two countries after I emigrated from England to New Zealand. The first two, Carmen’s Roses and Blue Moon for Bombers, appear separate from each other but the third, The Windflower Vibration, shows them to be linked. Three Novellas was described by one reviewer as “a superb trilogy finishing with an interesting twist”. The Kindle version (which can be read on any device not just on a Kindle) is on a free promotion until 2 July 2023 and you can find it on your local Amazon site.

- Jumping for joy

Ireland the Labrador greets me by jumping high in the air whenever I come to take him for a walk.
The two of us met about six years ago through The Dogshare Collective. One of his human family had suffered an injury at that time and needed help with his care. I started taking him out in the afternoons, and continued doing so long after his owner’s injury had recovered.
Ireland was bred to become a guide dog for the blind, but due to a minor defect in his own vision he was withdrawn from training and made available for adoption as a family pet. Large, friendly and exuberant, he loves playing with other dogs and like most Labradors he has an insatiable appetite. We have enjoyed many outings and adventures together (search the Animals section of my website to see illustrated posts about my walks with Ireland, also with my other dog share Buddy).
Having a dog brings great benefits – physical, mental and social – also involves great responsibilities. There are many people who are not in a position to have a dog of their own but would like to have a relationship with one. And there are many dogs who, often because their owners are out at work all day, need additional exercise and company. Within New Zealand The Dogshare Collective exists to put people from these two groups in contact with one another.
- On Rangitoto

Rangitoto viewed from Cheltenham Beach On a lovely sunny autumn day Brian and I visited Rangitoto, the volcanic island a short ferry ride from our home.

Disembarking from the wharf We walked up the steep track towards the summit.

Lava beside the track 
Auckland’s CBD in the distance When we last visited some years ago we made it to the top, but not this time. Not only do we have less stamina nowadays, but the upper parts of the track are quite hazardous after the recent floods. So we went back down and sat in the sun to eat our packed lunch (there are no cafes on the island). Afterwards we walked along the coastal path towards Islington Bay.

On the coastal path I was going to write a short description of Rangitoto, but thought AI might do it better. The following text was generated in a few seconds by ChatGBT.
Rangitoto Island is a volcanic island located in the Hauraki Gulf near Auckland, New Zealand. It is one of Auckland’s most iconic landmarks and a popular destination for tourists and locals alike.
Geology: Rangitoto Island is a volcanic cone that emerged from the sea around 600 years ago, making it one of the youngest islands in the Hauraki Gulf. It is part of the Auckland volcanic field, which consists of around 50 volcanic cones and craters scattered across the Auckland region. Rangitoto’s distinct symmetrical shape and its dark volcanic rock create a striking visual contrast against the blue waters of the gulf.
Natural Environment: The island is predominantly covered in dense vegetation, including native New Zealand flora such as pohutukawa trees, ferns, and shrubs. The pohutukawa trees, with their vibrant red flowers during the summer months, have earned Rangitoto the nickname “the Red Tree Island.” The island’s rugged landscapes and scenic trails provide opportunities for hiking and exploration, allowing visitors to experience its natural beauty up close.
Recreational Activities: Rangitoto Island offers various recreational activities for visitors. The island is accessible by a short ferry ride from downtown Auckland, making it a convenient day trip destination. Upon arrival, visitors can embark on walking tracks that lead to the summit of the volcano, offering panoramic views of Auckland’s skyline, the Hauraki Gulf, and the surrounding islands. Exploring the lava caves formed by ancient volcanic activity is another popular activity on the island.
Cultural Significance: Rangitoto holds cultural significance for the local Māori people, who consider it a sacred site. The island’s name, “Rangitoto,” translates to “Bloody Sky” in Māori, which is believed to originate from a historic battle that took place there. The island is home to archaeological sites, including Māori pa (fortified village) remains, which reflect its historical importance.
Conservation and Protection: Rangitoto Island is part of the Hauraki Gulf Marine Park and is managed by the Department of Conservation (DOC) in New Zealand. The DOC focuses on preserving the island’s natural environment, protecting its wildlife, and maintaining the integrity of its volcanic landscapes. Visitors are encouraged to respect the island’s fragile ecosystem by following designated tracks and leaving no trace behind.
Overall, Rangitoto Island offers a unique blend of natural beauty, volcanic history, and cultural significance. Its accessibility, diverse flora and fauna, and recreational activities make it an attractive destination for nature lovers, hikers, and those seeking a memorable experience in the Auckland region.
- Animal exports; a moral dilemma
A ban on the export of live cattle, sheep, goats and deer from New Zealand will come into force this month, following years of campaigning by the SPCA backed by widespread public support. But we are having a general election in October 2023, and the National and Act parties have stated that if they come into power, live animal exports will be started again.
This practice is both cruel and unnecessary. A position statement from the SPCA has described the stressors on animals undergoing sea voyages lasting weeks or months: fear and anxiety, exposure to disease, overcrowding, overheating, motion sickness and more. Some animals die on board, and in 2020 almost 6,000 drowned when a livestock container ship en route from New Zealand to Saudi Arabia sank off the coast of Japan. And, depending on the adequacy of health and welfare in the destination countries, animals may be subjected to further suffering when they arrive.
There are alternatives to live export. Animals for food could be slaughtered here and their refrigerated carcasses exported. For breeding purposes, semen and embryos rather than live animals can be used.
This issue presents me with a moral dilemma. I don’t want to see the Labour Party returned again; since they have been in government New Zealand has gone backwards with falling standards in healthcare and education, increased poverty and crime, increased racial divisions, billions of dollars wasted on idealistic projects which have never been completed. Until now I had been firmly intending to vote for either National or Act, but how can I justify supporting a party which will reinstate live animal exports? Several letters published in the NZ Herald newspaper, including one from me, have expressed this dilemma. I have written to the party leaders, and my local MP, to protest the policy and I hope that if enough other people do the same they will revoke it. If not, is the only answer not to vote at all?
- Books I’ve enjoyed #13
The current interest in issues of gender identity prompted me to read Radclyffe Hall’s autobiographical novel The Well of Loneliness, which was banned after its publication in 1928 but is now regarded as a classic. It is about a girl born in the late Victorian era to a wealthy family living on a country estate near Malvern. Despite being biologically female, ever since early childhood her appearance and behaviour has been obviously masculine. Although her parents feel greatly puzzled and concerned by her condition they never speak of it. When she grows up and falls passionately in love with another woman, her mother is forced to acknowledge her nature, and rejects her as “a sin against creation”. During later life in London and Paris she achieves success as a novelist and forms a loving relationship with a younger woman, but is eventually unable to withstand society’s condemnation of “inverts”. Nowadays her condition would be more widely accepted and she would be a candidate for sex reassignment surgery. This sad book contains sensitive descriptions of the main character’s tribulations, and of English country life as it used to be.
I listened to the audiobook version of Prince Harry’s memoir Spare. It is well written (by a ghost writer) and Harry narrates it fluently, He comes over as a fun loving but often troubled man whose most positive experiences have been his army service, his charity work with wounded veterans, and falling in love with Meghan. Although the text contains plenty of interesting material, it is pervaded by the author’s sense of victimhood, entitlement, hatred of the press and resentment towards the royal family. I feel these attitudes can only partly be justified by the trauma of losing his mother when he was eleven years old, terrible though that must have been. We await the next episodes of his life story.
Clare Chamber’s novel Small Pleasures is set in the suburbs of London during the 1950s. Jean is a middle-aged unmarried woman who works as a journalist on a local newspaper and lives with her demanding elderly mother. Her drab existence is enlivened after she begins research for a feature about a young girl who is allegedly the product of a virgin birth. The details of Jean’s domestic life, and the development of her character as she becomes emotionally involved with the girl and her parents, are engagingly described in a style reminiscent of Elizabeth Taylor or Barbara Pym. It must have been difficult to devise a satisfactory ending to the story and the last few chapters are not up to the standard of the earlier ones. Despite this criticism I very much enjoyed the book.
- Books I’ve enjoyed #12
Girl, Woman, Other by Bernadine Evaristo, which won the Booker prize in 2019, is a series of vignettes about 12 women, mostly black lesbians in London, whose lives intersect. There is no punctuation and in parts the writing resembles free verse rather than prose. Neither the style nor the subject would normally have appealed to me, but having been given this book as a gift I felt obliged to read it, and was surprised how much I enjoyed it.
Kate Elizabeth Russell’s semi-autobiographical novel My Dark Vanessa has attracted much controversy, with one reviewer calling it tragic, repulsive and infuriating. As a 15-year-old schoolgirl in Maine, the narrator willingly entered into a sexual relationship with her 40-something English teacher. Their affair continues to impact her life many years later, especially in the light of the MeToo movement. It would be far too simplistic to describe this psychologically complex situation in terms of victimhood, abuse or even rape. A challenging but absorbing read.
Turning from books about the intricacy of sex and gender issues in today’s world to a refreshingly straightforward memoir of wartime service. A Spitfire Girl by Mary Ellis describes the work of the ferry pilots in the Air Transport Auxiliary, who transferred aircraft between RAF bases in World War Two. This remarkable woman flew over a thousand planes of 76 different types, ranging from Spitfire fighters to Wellington bombers. After the war she continued a long career in aviation, and died in 2018 at the age of 101.
I was feeling guilty about never having read Middlemarch by George Eliot, published in 1871 and widely considered the best English novel of all time, so I bought myself a copy for Christmas. I can see it is a monumental achievement, but with so many long descriptive paragraphs I am finding it hard going and have given up my intention of reading one chapter per day. I think this shows how much writing styles have changed over the years, also how my own attention span has got shorter presumably due to continual use of electronic devices.
I’ve been reading some lighter modern novels as well and will mention just a few. Small Things Like These by Claire Keegan is an elegantly written, quietly disturbing short book set in the 1980s in a rural Irish community dominated by the Church. The Lamplighters by Emma Stonex, inspired by a real event, is about the disappearance of three men from a lighthouse off the Cornish coast in the 1970s, and how the unsolved mystery continues to affect their wives many years later. Lastly, being a fan of psychological crime stories set in Oxford, I am enjoying Ruth Ware’s The IT Girl . A man serving a sentence for the murder of a college student ten years earlier has died in prison – but was he guilty after all?
- Two dogs
Although I don’t have my own dog, I have the pleasure of knowing several local ones, and regular “dog sharing” arrangements with two of them: Ireland the Labrador and Buddy the Cavoodle. This involves taking them for walks, and sometimes keeping them company while their owners are out. I love both dogs equally, but they are so different from one another it can be hard to believe they belong to the same species, canis lupus familiaris.

Ireland the Labrador Ireland is a confident, exuberant big black Labrador nearly six years old. He loves everything life has to offer: going for walks, playing with other dogs, riding in cars, and most of all he loves eating – almost anything except kidneys. His only fault is a tendency to bolt towards any source of food, such as a picnic or a discarded pie, which he can smell from far away. I have been walking him for about four years now and his joyful greeting when I come to see him always makes my day.

Buddy the Cavoodle Buddy, a second generation Cavoodle just coming up to his first birthday, is a more sensitive soul and prone to anxiety even though he has been raised with the utmost kindness. He is gradually becoming more confident, and now enjoys going for walks although he was previously reluctant to leave the house. He still hates car travel, and in further contrast with Ireland he is indifferent to food, and often has to be coaxed into eating. Buddy is a very handsome dog, with an affectionate nature. He loves cuddles and is still small enough to sit on my lap.
The characteristics of Ireland and Buddy are typical of their respective breeds. For example it is well established that Labradors are obsessed with food, and that Cavoodles are prone to separation anxiety. Although the way that dogs are treated and trained has a big influence on their development, research has shown a clear genetic basis for inter-breed differences in personality, behaviour and intelligence. https://theconversation.com/genetic-research-confirms-your-dogs-breed-influences-its-personality-but-so-do-you-196274. Doing similar research on humans would be considered racist and unethical nowadays.
- Thoughts on later life
“…we believe a full life is one that gets richer with age … rediscovering lost passions and plunging headfirst into new ones … embracing new experiences … bringing joy and meaning to every moment.” This is a shortened version of the text on the website of Ryman Healthcare. Is it realistic to expect old age, whether or not in a Ryman retirement village, to be so idyllic? Or is it more likely to be dominated by adversities such as loss of health and vitality both mental and physical, lack of occupation, reduced income, bereavement, loss of status, social isolation, and the prospect of death whether feared or welcomed? I expect it depends a lot on individual attitude.
Quite a number of my own contemporaries have died before reaching old age, having for no apparent reason developed some fatal disease, usually cancer. Others are still alive and during my recent holiday in England I had the pleasure of renewing friendships with some of those I have known for a long time – from high school, medical school, or hospital jobs in Southampton and Oxford. Since coming back home I have also met up with my New Zealand friends. Our conversations often touched on the question of how to adjust to retirement.
Almost all of us, in our 70s or 80s, have the good fortune to be living in comfortable circumstances with reasonably good health, family connections and ample money, allowing plenty of choice about how to spend our free time after leaving paid employment. My friends described a wide range of activities including charity work, looking after grandchildren or animals, gardening, travel, socialising, entertainments, reading, writing, cooking, painting, crafts, sports, fitness classes, music, academic study, spiritual practice.
Everyone seemed fairly content, especially those who were pursuing some compelling interest, or simply enjoying the freedom to relax and do just what they liked. Others, more introspective, found their lifestyle pleasant enough but questioned whether they were making the best use of whatever time might remain. Some were missing former jobs which had involved contributing to society and being recognised for it. They had not been able to find a type of voluntary work which made full use of their abilities and experience.
One woman who is highly artistic stated that the most vital thing was to express creativity, if only for oneself. I agreed that creativity is very important but felt that the resulting products should be shared with others. There is an example of these differing views at home, where my husband and I both spend a lot of time writing. He does it primarily for his own satisfaction and does not care much whether anyone else ever sees it. In contrast, I like to publish my work in the hope that some readers will benefit from my medical books or enjoy my novels – while trying not to be too flattered by good reviews or too upset by bad ones, for the Stoic philosophers advised against seeking appreciation. They said that the best way to live – at any age – is by striving to be a good person, and focusing only on things you control.
- Books I’ve enjoyed #11
Many books have been written about the Second World War, but there always seems room for more, and my two non-fiction choices for this post provide entirely different perspectives. The Splendid and the Vile by Erik Larsen is an extensively researched account of Winston Churchill’s first year as wartime prime minister, 1940-41. I found the book very easy to read, partly because the detailed information about political and military events is brought to life by personal insights from the diaries of Churchill’s daughter Mary, his private secretary John Colville, and members of the Mass Observation project. Even though Churchill had his flaws and made some decisions which proved misguided, it is impossible not to admire his tremendous energy and stamina, his optimism and determination, his skills as a leader and orator which inspired the British people during the darkest days of the war.
In complete contrast is the extraordinary book When I Was Someone Else by a French journalist, Stephane Allix. During a spiritual retreat in Peru, Allix had a vision of a German soldier dying on a snowy battlefield, followed by scenes from the man’s life, and including his name. Allix became obsessed with this vivid experience, and from military archives discovered that a soldier of that name had served in the brutal Totenkopf division of the Waffen SS, and been killed during the 1941 Russian campaign. Allix was able to contact surviving relatives of the dead man and discover facts which corroborated the content of his vision. Having first assumed that the vision represented a past life of his own, Allix later concluded this was not so, but that the soul of the dead soldier had contacted him in search of forgiveness and healing. I did not know quite what to make of this book, but it will be of interest to students of paranormal phenomena such as reincarnation and spirit communication.
Turning to fiction, as usual I’ve been reading mainly mysteries and psychological thrillers, and I’ll mention two of them which were written by health professionals. Deadly Cure by Mahi Cheshire is about the rivalry between two young female doctors competing for a job at a research institute developing a vaccine against cancer. When the successful candidate gets murdered, suspicion falls on her rival. Some of the medical content is not credible, as the author – herself a doctor – would no doubt admit. But dramatic licence is allowable in fiction, and as light entertainment I found this short book quite gripping.
More grounded in grim realism is The Family Retreat, by clinical psychologist Bev Thompson. The story is narrated by a burnt-out GP who, with her young family, rents a summer holiday cottage near the Dorset coast. She makes friends with another woman who has children similar in age to her own, and they share some pleasant seaside picnics until a dark secret is revealed. This is a rather sombre read, with much reference to mental disorders and troubled relationships, and constant soul-searching by the narrator raising such questions as how far doctors should take responsibility for their patients’ lives, and why so many women submit to being imposed upon by men.
- Two countries
With New Zealand’s borders open again I have been able to make another trip to my home country of England, after a gap of over three years. Being in London when the Queen died, and during the subsequent period of national mourning, was a truly remarkable experience.
Sadly there wasn’t enough time to see all of my relatives and friends living in various parts of the kingdom, but I did visit a lot of places, too many to list here. I stayed several days in Oxford, where I did my medical training and spent much of my career, meeting some old colleagues and exploring the riverside and surrounding water meadows.

Grandpont, Oxford One day I took the train to Malvern, with its memories of Elgar’s music and my time at the College of Healing. The town features in my novel “The Windflower Vibration”. I walked up the hills and had tea at St Anne’s Well.

On the Malvern Hills Another highlight was staying with an old school friend who lives in a converted farmhouse in Wharfedale, Yorkshire. We walked the dogs by the river, and ate fruit from the orchard where 250 apple varieties are grown.

Washburn river 
Apple orchard For the first few years after I moved to New Zealand in 2000 it seemed easy enough to make frequent return trips to the UK. But international flying has become much more complicated and expensive since the pandemic, and attracts increasing criticism for its impact on the environment. Also, having reached a later stage of life, I wonder how much longer I will be fit to travel. So although I hope this latest visit to England won’t be my last, I am aware that it might be.
Knowing this I do sometimes feel torn between my two countries. But my present life in Auckland is a very happy one, and over the years I have enjoyed the best of both worlds.
.
- “No good deed goes unpunished”
Actions intended to benefit other people sometimes backfire. They may be perceived as interfering and controlling, or even have tragic results.
I’ve been thinking about this since watching a brilliant performance of Verdi’s Il Trovatore by NZOpera and the Auckland Philharmonia Orchestra. In the melodramatic plot, set in fifteenth century Spain, Count di Luna is obsessed with the heroine Leonora. But she is in love with Manrico the troubadour, and spurns Luna’s advances. There is bitter rivalry between the two men and eventually Luna gets Manrico imprisoned and condemned to death. Leonora, in what she sees as a noble sacrifice, offers herself to Luna if he will spare Manrico’s life. But when Manrico learns of Leonora’s plan, instead of being grateful he is disgusted and appalled, and denounces her. Meanwhile, rather than give her body to Luna, she has taken poison. Manrico is executed, and Leonora dies.
The old adage “No good deed goes unpunished” often applies in real life. During 2020 and 2021, the New Zealand government responded to the pandemic by imposing a strict system of lockdowns, mandates and border closures to protect the health of the population. These well-intentioned policies did limit illness and death from Covid in the short term, and gained admiration from around the world. But were they justified when weighed against the long term costs? Businesses failed, unvaccinated workers lost their jobs, other diseases went undiagnosed and untreated, old people were confined indoors and prevented from seeing their relatives even when they were dying. Despite continual exhortations to “be kind”, ugly rifts developed between those who supported the restrictions, and those who resented losing the freedom to direct their own lives.
On a more everyday level, think of the dinner guest who volunteers to do the washing up, only to put things away in the wrong place and break the host’s favourite mug.
My conclusion? It’s good to offer help to other people – but only if it’s done with unselfish motives and if they want to be helped.
- Buddy the beautiful Cavoodle

Buddy aged 8 weeks I’ve just met my new dogshare puppy, Buddy. I will be helping to look after him on days when his owner cannot take him to work. He is a lively, cuddly and confident little pup and I fell in love with him at first sight.
A Cavoodle is a cross between a Cavalier King Charles Spaniel and a toy or medium Poodle. Such dogs, weighing 4-12 kg, are said to be very affectionate, energetic and intelligent. Apparently they love human company, being prone to separation anxiety when alone; are not especially keen on food (what a contrast to my Labrador dogshare, Ireland); and are good swimmers.
Buddy is a 2nd generation cross, from two Cavoodle parents, and through the genetic lottery appears to be more Spaniel than Poodle. He looks very like a Blenheim Cavalier King Charles Spaniel – chestnut and white, with a “Blenheim spot” on the top of his head. According to the Wikipedia site about that breed: “The Blenheim spot is also known as the mark of the Duchess Thumb Print, based on the legend that Sarah Churchill, Duchess of Marlborough, while awaiting news of her husband’s safe return from the Battle of Blenheim, pressed the head of an expecting dam with her thumb, resulting in five puppies bearing the lucky mark after news that the battle had been won.”

Buddy aged 9.5 weeks Dogsharing involves dividing both the joys and responsibilities of dog ownership between households, in a flexible way arranged on an individual basis, for the benefit of both the humans and animals concerned. Within New Zealand, matches can be arranged through the Dogshare Collective.
- Memoirs of an Oxford medical student 1967-70

Osler House, Woodstock Rd More than 50 years after graduating from Oxford University Medical School, I found a boxful of letters and diaries which I had written during my clinical course. To a naive 20-year-old from a rather sheltered home background, whose first degree at Leeds University had involved more work than play, life in Oxford was a revelation – intellectually, socially and emotionally. My memory for the past is fairly patchy and though I clearly recall some of the people, places and events described, I have forgotten many others which were obviously significant at the time. I was known by my maiden name, Jenny Collins.
The course was mainly based at the old Radcliffe Infirmary in Woodstock Rd. For some attachments we visited the Churchill Hospital, where I would later become a junior doctor and eventually a consultant, Cowley Road Hospital, and the Nuffield Orthopaedic Centre. The Radcliffe Infirmary was closed in 2007 and its site is now occupied by university offices. The hub of student life was Osler House (not to be confused with the present clubhouse of the same name on the John Radcliffe site) an 18th century listed building in the hospital grounds. Downstairs was a lounge, bar and kitchen. Morning coffee and afternoon tea were provided free. Upstairs were bedrooms for use when on call. There was an attractive garden with a croquet lawn. Each student also had an attachment to an Oxford college – mine was Somerville – but being postgraduate did not live in. My first few months were spent lodging in Summertown with the mother of a family friend, the widow of a bishop and a keen supporter of Moral Rearmament. After I had moved into my own flat, my former landlady continued to invite me for dinner on Sunday evenings.
Our intake contained only 18 or 20 students. Being divided into even smaller groups for clinical attachments, we got a great deal of individual attention from our teachers. For me, as one of the few women in a male-dominated environment, this was often of a kind which would not be tolerated nowadays. As well as clerking patients we were given considerable responsibility for practical procedures such as taking blood, putting up drips, lumbar punctures, delivering babies, and assisting with surgical operations.
There were periods of intense activity – on take for medicine and surgery, night deliveries in obstetrics, preparing for exams. But otherwise the pace of work was fairly leisurely and allowed time for a vibrant social life. Lunches, dinners, parties and outings were frequent and usually involved vast quantities of food and drink. I sang in the hospital choir and in my final year played a good fairy in the students’ pantomime, Tingewick. I must have done a certain amount of studying but most of my free time seems to have been spent entertaining friends for supper or afternoon tea, making my own dresses, listening to pop music, or walking around Oxford which was then a peaceful place with few cars. Several of my friends did have cars, and when they were driving north would give me lifts home at weekends. It was a privileged and mostly hugely enjoyable life which, I imagine, was far more relaxed and informal than for clinical students today.
Much of what I wrote is too trivial, personal or libellous to publish, but maybe I will adapt some extracts for a series of blog posts, a memoir of a novel. Meanwhile I’d be pleased to hear from anyone who remembers those times.
- On the other side of the (medical) fence
Since retiring from medical practice I’ve exchanged the role of doctor for those of patient and of patient’s wife, and being on the other side of the fence has been an interesting experience. Between the two of us, my husband and I have needed to see a good many different healthcare professionals from various specialties in recent years. Most of them were excellent, but a few were unsatisfactory and this was usually because of their poor “communication skills”.
Following the retirement of the family doctor we had known and trusted for a long time, I saw a GP whose failings included a rude manner, ordering me to take a long-term prescription for a new drug without any discussion of its efficacy and side-effects, and – as I discovered later – referring me to a hospital clinic without telling me. After that I changed to a different practice and am very happy with my doctor there, but my experience with the previous one distressed me for a long time, illustrating the importance of a good therapeutic relationship not only for improving patients’ emotional well-being, but for influencing their compliance with treatment and the outcome of their disease.
I don’t remember having any guidance about how to relate to patients when I was at medical school in the 1960s, nor during my junior doctor posts. Senior role models varied greatly in their approach, ranging from the caring and compassionate to the arrogant and disrespectful. In the later years of my career this aspect of clinical practice began to be taken more seriously, led by specialties such as general practice, oncology and palliative care. Communication skills training is now included in the education of doctors, nurses and other healthcare professionals, though its long-term impact must be difficult to measure, and depend on the student’s personality. The skills may come naturally to those who have chosen their career for humanitarian reasons. Those who are mainly interested in the scientific and technical side, or whose prime objective is making money, may pay little attention to such “soft” subjects in the curriculum.
The basic principles should be obvious, simply involving courtesy, common sense and genuine concern for the patient. Giving a polite and friendly greeting. Meeting in a clean and tidy consulting room free of interruptions. Listening to the patient’s story with genuine interest and empathy. Taking account of the patient’s knowledge and preferences when discussing management of the problem.
Conducting the interview becomes more difficult in the case of a serious condition. The medical literature contains many studies about techniques of “breaking bad news”, usually in relation to a cancer diagnosis, and I won’t attempt to detail them all here. Key points include giving truthful information without destroying hope. And avoiding dogmatic statements about prognosis, because the outcome in individual cases can vary so much from the average. Negative predictions can be self-fulfilling as well as disheartening, whereas except in the most dire situations there is always some help to be offered, and some scope for improvement. Another point highlighted by our recent experiences is that illness can be just as stressful for relatives as for patients themselves.
- Ireland visits Normanton Reserve (“not” Devonport Dog walks #5)

Ireland in Normanton Reserve Although I’m including this post in the Devonport walks series, it actually relates to a different part of Auckland. This is because Ireland, the dogshare Labrador I’d been walking most afternoons for four years, has moved out of the city with his owners’ family. Contact is less frequent now, but our bond continues unbroken, and Ireland greeted me ecstatically when we met halfway for a visit to the Normanton Reserve in the Wairau Valley suburb.
I had driven around there many times in the past for business purposes, not for pleasure because it is a rather unattractive industrial area prone to traffic congestion. I had no idea there was a peaceful green reserve close by, hidden away at the end of a cul de sac.

Lower field 
Playground The large flat grassed field on the lower level of Normanton Park offers activities for both adults and children. On the path that encircles the perimeter there are a series of exercise machines – I did not try these. There is a playground, a small basketball court and a small skateboarding park, a picnic area and toilet block, all clean and well maintained.
On an upper level, reached by a short flight of steps, is a large field in a more natural state with plenty of room for a dog to run free.

Upper field Ireland’s departure has been a loss but I will certainly keep in touch with him and meanwhile, with other local dogshare opportunities on the cards, have had the gaps in our garden hedge sealed off …

A puppy-proof fence - Waiheke interlude
Brian and I spent two days on Waiheke Island, staying in a comfortable and spacious holiday home surrounded by native bush and overlooking the sea. Though New Zealand’s summer is nearly over, the weather was sunny and hot. Waiheke has a semitropical climate, lush vegetation, sandy beaches, boutique vineyards and olive groves, a friendly and somewhat bohemian vibe, and feels a world away from the mainland.

Huruhi Bay viewed from the balcony Except during Auckland’s lockdown periods we have often made day trips to Waiheke. The 40-minute ferry ride from the city centre, across a calm blue sea flanked by other small islands, always induces a sense of relaxation. Parts of my novel Cardamine are set on Waiheke and this extract contains some references to the history and geography of the island.

Waiheke Island. Source: Wikipedia Waiheke holds many memories for me, some bittersweet. Stonyridge Vineyard has been our usual venue for birthday and anniversary lunches. Our group of local Bach flower remedy practitioners, now depleted by the loss of key members, has held weekend gatherings in more modest settings such as the Quaker meeting house. The sad story of my first rescue cat, Orange Roughy, had a happy ending when he was successfully rehomed on the wild far reaches of the island.
During this recent short holiday we went swimming at Palm Beach, climbed up and down a steep track for coffee and galettes in Bisou cafe at Surfdale, dined at Vino Vino and The Courtyard in Oneroa.

Palm Beach - My Author Bio
I have just turned 75, and it feels like the right time to review my long and winding journey to becoming an author.
Writing was my first love and as a child growing up in Kent I produced a variety of short stories and plays. These early works have long since been thrown away and their content forgotten, though I think they usually featured cats and dogs. I did well in English at school and was expected to take a university degree in that subject, but in my teens I developed an idealistic wish to heal the sick. The medical courses at Leeds and Oxford, then life as a junior doctor, absorbed so much time and energy that I never even thought about writing fiction again till years later.
It was after many changes both professional and personal that I decided on a career in psychiatry, and when studying for the postgraduate qualifications I compiled my notes into what would turn out to be my first book. A senior colleague suggested sending it to a publisher. It was accepted, and without any marketing on my part sold well and continued into five editions; by far my greatest commercial success. I moved on to academic posts, involving opportunities for research, writing papers for journals, and medical books relevant to my specialty of the interface between psychiatry and cancer.
In my mid-30s, when finally settled into a contented domestic life, I wrote three novels inspired by my earlier work experience in general practice and in mental hospitals. I enjoyed this tremendously, and given my earlier success with the psychiatry book, I assumed that I would have no trouble getting them published. I was soon disillusioned. Some rejection letters were encouraging but others were not, and I was so upset by one damning verdict that I put the manuscripts aside for 20 years. An overreaction, and I now realise that you can’t please everyone and that even the best of books gets an occasional bad review. Knowing how devastating it can be for writers to receive harsh criticism of their work, I will only review a book myself if I can give an honest positive opinion.
Fast forward to my 50s when, after a rewarding career as consultant in psychological medicine in Oxford, I came to live in New Zealand. Alongside many new interests, I focused on writing and editing. Twenty years later I have a variety of titles, non-fiction and fiction in a variety of genres, some traditionally published and some under my independent imprint of Overcliff Books, listed on my Amazon.com and Amazon.co.uk author pages. My current project is editing my husband’s autobiography. What, if anything, I will write next I don’t know.

- Books I’ve enjoyed #10
I had plenty of time for reading during Auckland’s prolonged lockdown and the very hot summer which followed.
First, some popular novels set in the UK. The Rose Code by Kate Quinn, about three young women who worked as code-breakers at Bletchley Park during World War Two, is an intriguing and well researched combination of fact and fiction. Watch her Fall by Erin Kelly is a complicated story which gives insights into the world of ballet, and after reading it I will watch Swan Lake with new eyes. The Black Dress by Deborah Moggach, an elderly woman’s quest to find a new man after being deserted by her husband, is full of dark humour and was described in The Times review as a “deliciously savage tale of sex and death”. And Greenwich Park by Katherine Faulkner is a psychological thriller in which a pregnant woman’s life is disrupted by the stalker she meets at an antenatal class.
Next, a small selection of the many books recently published by members of the Auckland Crime Writers group. Blood on Vines by Madeleine Eskedahl, Quiet in her Bones by Nalini Singh and my own novel Cardamine are all set in New Zealand and evoke the local scenery of forests, beaches and vineyards. Some describe other locations. The Girl in the Mirror by Rose Carlyle is set on a yacht, and The Forger and the Thief by Kirsten McKenzie is a historical thriller set in Florence.
Two novels in the literary fiction genre. Klara and the Sun by Kazuo Ishiguro, narrated in the voice of a gentle and observant robot who is purchased as the “artificial friend” of a fragile teenage girl, is a readable story which raises some profound questions. More challenging is We Germans by Alexander Starritt, in which an old man writes to his grandson in an attempt to come to terms with his past as a soldier serving on the Eastern front in World War Two.
Four non-fiction books which left an impression on me. The Devil You Know by Gwen Adshead and Eileen Horne contains a series of (disguised) case histories of psychotherapy with mentally disturbed criminal offenders, not all of whom could be helped. I reread an older book, The Power of Premonitions by Larry Dossey, a physician who has made a detailed study of “psi” phenomena. Against All Odds by Craig Challen and Richard Harris is a vivid description of the 2018 rescue of the young boys trapped in a cave in Thailand. Lastly, Dear John by Joan Le Mesurier is about her marriage to the actor who is still fondly remembered for his role as Sergeant Wilson in Dad’s Army.
- Fostering kittens again

Photo by little plant on Unsplash It’s been a long time since we last had foster cats or kittens in the house, the reason being that I’ve usually ended up adopting them permanently. Having promised my husband that won’t happen again, last week I took in two more from a local animal welfare charity. It’s against the rules to post their photos online so I’ve used a stock image.
My first experience of fostering in New Zealand, over twenty years ago for a different charity, was quite informal. A litter of four small kittens was delivered to the door and I was left to get on with caring for them until they were old enough to be adopted. I kept one, Felix, a dearly loved cat as described in this post.
Nowadays, the role of a feline foster parent is much more tightly controlled. The online application process requires obtaining a criminal history check, answering multiple-choice quizzes based on the content of a 30-page manual, and submitting photos of the proposed foster room setup. After completing it successfully, I got a call from the volunteer coordinator and arranged an appointment to drive out to the nearest rescue centre.
I returned home with two kittens, a black male and a tortoiseshell female. They are about 10 weeks old and before being made available for adoption they will need to complete medication for an intestinal infection, receive worm and flea treatments and vaccinations, and gradually transition to a different diet. Looking after them involves providing fresh food and water, changing litter trays, and sessions of play and cuddles every few hours. I am also giving extra attention to our two adult cats who are being strictly kept apart from the kittens but are keenly aware of their presence. Leo seems frightened of them whereas Magic seems hostile.
Fostering these kittens is a big responsibility and time commitment, but also a delight, because they are as lively and affectionate as can be and it’s going to be hard to give them up.
- A canine memorial service
A group of dogs who were bred in Auckland’s Guide Dog Centre meet every week for a “play date” in one of our local parks. Most of them are Labradors, either black or yellow. They include puppies in training, working dogs both active and retired, and those who were withdrawn from the training programme and are living as family pets. I was introduced to this group through Ireland, a four-year-old black Lab in the “withdrawn” category, who is owned by a local family. I am his “dog-sharer” who walks him almost every afternoon, as described in a series of my recent blog posts.
Three of the long-term canine members of the group have died in recent months. Two of them were near the end of their natural lifespan, which for Labradors is 10-12 years. The third, who was a little younger, had developed heart failure. Today we gathered in a beach-side reserve to honour their memories. The weather pattern of sunshine and showers mirrored the bittersweet mood of the occasion. There were tears as each of the bereaved owners delivered a short eulogy to their dog, but there was pleasure in sharing food and drink with friends while watching the younger Labs chase each other round the grass and jump into the water. Like a human memorial service, it was a significant event.
When I lived in England I volunteered with the Society for Companion Animal Studies (SCAS) to provide telephone support to people who were distressed by the loss of a pet. Through that work, as well as through my personal experience, I learned that the death of a beloved companion animal can be no less devastating than a human bereavement. Those who do not love animals find it difficult to understand grief of such intensity, and may make hurtful remarks like “It was only a dog” or “Why don’t you just get a new one”. A lost pet cannot simply be replaced in the same way as a worn-out garment or an old car. Having said that, many owners will find comfort by bringing another animal into their homes when they feel ready to do so.
- New Zealand Mystery ‘Cardamine’ by Jennifer Barraclough
New Zealand Mystery ‘Cardamine’ by Jennifer Barraclough http://thoughtsbecomewords.com/2021/11/17/new-zealand-mystery-cardamine-by-jennifer-barraclough/ — Read on thoughtsbecomewords.com/2021/11/17/new-zealand-mystery-cardamine-by-jennifer-barraclough/
- Ireland visits Mt Cambria (Devonport dog walks #4)

To quote from a local tourist website: “Mt Cambria Reserve is quiet retreat in the pretty seaside town of Devonport. The attractive landscaped garden sits in the remains of Mt Cambria volcano, which was a quarry for scoria rock between 1883 and 1985. Mt Cambria Reserve is situated behind Devonport Museum on 31a Vauxhall Road and is an ideal spot for walks and relaxing picnics.”

Ireland can smell a picnic Ireland has to be kept on a tight lead when picnics are in progress – like most Labradors he has an insatiable craving for food. But provided there are no picnics, Mt Cambria is a lovely place for dogs to run free. It’s quite a small park, dotted with clumps of trees, and has a steep slope at the back.



Ireland rolling down the grassy slope From the top of the park is a view of Mt Victoria, another good place for dog walks as described in an earlier post.

A highlight of Ireland’s week is his “club day” when he spends an hour rushing around Mt Cambria with a group of his canine friends while their owners look on.

- Writing as an Englishwoman in New Zealand
Here’s a little background to my new novel Cardamine: A New Zealand Mystery. Amazon links: US, UK, AU

Most novels contain elements of autobiography and the setting for this one was informed by my own memories of visiting New Zealand for the first time, discovering the beautiful beaches and countryside, the enticing vineyards and coffee shops. Several North Island locations – Waiheke, Browns Bay, Riverhead Forest, Muriwai – are featured in the book. There are also references to the confusion that can arise from subtle differences in culture and use of language between two English-speaking nations. My background in medicine and psychiatry had an influence on the plot, with speculation about how emotions, beliefs, personality factors and mental or physical illness can contribute to crime.
The main character, Kate, is in New Zealand on holiday on the eve of the Covid-19 pandemic. She is much younger and more adventurous than me but shares my liking for sea swimming and the local wines. After drinking rather too much of them during a vineyard tour, she loses the bag containing her valuables and so misses her night flight back to London. A rich and eccentric elderly man comes to her rescue and invites her to stay in his country house, called Cardamine after the flowers around the pond in the garden. His wife, a “mail order bride”, is mysteriously absent. Kate’s summer holiday had begun as an idyll of sunshine and swimming and budding romance, but she becomes aware that the country’s “clean green” image conceals a darker side involving racial prejudice, illegal drug use and unnatural death.
Cardamine is available in paperback or Kindle format from your local Amazon website: US, UK, AU. New Zealand residents can buy a print version directly from me – please write via my contact page if you’d like to order a copy.
- Free speech?
“This may be offensive to your reader” warns Microsoft Word when it finds bitch in the text of my forthcoming novel. Considering that I was using the term to describe a female dog I find this quite amusing, but it makes me think about other less trivial ways that the use of language is becoming curtailed. One of my characters expresses racist views before being admonished by his wife, and I understand that a similar incident in one of Sally Rooney’s books led a journalist to accuse the author herself of racism. JK Rowling was “cancelled” for a comment that some interpreted as transphobic – fortunately my novel contains nothing about gender identity issues. It seems more acceptable to portray violence towards people and animals in fiction than to risk upsetting “woke” sensibilities.
Free speech is also limited in real life. Here in New Zealand, doctors who express valid concerns about the safety of Covid vaccination are being disciplined by the medical authorities. The rare but well authenticated cases of serious illness or death attributable to this vaccine are seldom reported in the media, and campaign materials designed to get everyone vaccinated make no mention of potential risks. I regard the vaccine as the lesser of two evils so have had my own two shots, but I respect the rights of those who have researched the pros and cons of this intervention and decided not to accept it.
- Ireland visits Mt Vic (Devonport dog walks #3)
Ireland the Labrador loves walking up Mount Victoria/Takarunga, known by Devonport locals as Mt Vic. Of unknown age, it is the tallest volcanic cone on Auckland’s North Shore, though being only 87 metres high it is really a hill rather than a mountain. The wooded lower slopes are surrounded by old houses, churches and a primary school and there are several access points.

Mount Victoria viewed from Cambria Park We usually approach the site through the historic cemetery, dating from the late 1800s, where the Maori warrior and peacemaker Patuone is buried alongside early white settlers.

Mount Victoria cemetery Mt Vic was once a Maori pa (fortified settlement) and the remains of old terraces and kumara pits can be seen alongside the walking tracks that now encircle the site. Ireland seems fascinated by the place and sometimes, perhaps drawn by sights or smells or spirits of the past, he dashes up the steep grassy hillside and on one occasion took half an hour to return. At other times he freezes on the path as if hypnotised.

Ireland transfixed On the summit, with its panoramic views of Rangitoto, the Hauraki Gulf, Waitemata Harbour and Auckland’s CBD, are various modern structures: mushroom-shaped vents for an underground reservoir, a signal station for shipping, a disappearing gun. There are a few older military remains on Mt Vic and a delapidated army hut, known as the Bunker, is the venue for the local folk music club.

The Bunker After completing the steepest part of the walk, Ireland and I stop for a rest and a snack.

Ireland hoping for another biscuit - Ireland visits a maze (Devonport dog walks #2)
Last week I wrote about taking Ireland, my dogshare Labrador, to North Head. Another of our favourite places to walk around Devonport is Ngataringa Park. Developed in the 1990s from an old landfill site, this is not a formal park but mostly consists of large fields which provide an ideal space for dogs to run and play and roll in the long grass.

Various local landmarks can be seen from the curved path that runs through the park. Auckland’s harbour bridge, viewed from across the tidal estuary with its mangrove swamps. Mount Victoria, or Takarunga – the highest volcanic cone on the North Shore – and another good place for a dog walk. The massive new retirement complex being built on a nearby hill overlooking the site. There is a skate park in one of the fields, and a piece of artwork, a pair of wooden statues called The Guardians.

At the far end of the path is a maze, intended to represent the interweaving between Maori and Celtic cultures. Beside it, a network of small circular paths bordered by stones is hidden in a group of trees. This is the halfway point of our walk, and while I have a rest on one of the rustic seats made of driftwood, Ireland eats a few biscuits and then waits patiently at my feet.

We can either go back the same way that we came, across the fields, or take the lower path which is shaded by an arch of trees.

- Ireland visits North Head (Devonport dog walks #1)
As Auckland’s lockdown continues and we are told to stay within our own postcode area, the highlight of my daily routine is a walk with my dogshare Labrador, Ireland. There are several interesting places nearby and one of our favourites is the hill called North Head, or Maungauika, which forms a prominent landmark at the end of the Devonport peninsula.

Dogs are permitted here – on lead The hill is encircled with a network of paths and from the higher ones there are spectacular views of Cheltenham beach to the north, Rangitoto and the islands of the Hauraki gulf to the east, the Waitemata harbour and Auckland’s CBD to the south. It was a wonderful location for watching the yacht races during last summer’s Americas Cup.

Cheltenham beach 
Rangitoto North Head was formed by a series of volcanic eruptions about 50,000 years ago. About 1,000 years ago it became occupied by a Maori tribe, then after European settlers arrived was put to use as a coastal defence site. During the late 19th century a number of large guns were installed to deter a feared Russian invasion. Fortifications including more guns, searchlights, tunnels and underground rooms were added, using prison labour, to cope with subsequent threats during the two world wars. The army left the site in the 1950s but a naval training school remained on the summit until 1996. The site is now managed by the Tupuna Maunga Authority and open to walkers and their dogs (on lead).

One of the many guns on North Head Remains of the old military installations can be seen around the site. Some of the tunnels are open to the public, others shrouded in mystery and rumoured to contain aircraft or military secrets. At present however all the tunnels are closed due to Covid restrictions, as is the colourful toilet bock.

Ireland denied access to tunnel 
The toilet block I find North Head a fascinating place which carries an air of mystique. It features in Carmen’s Roses, the first short novel I wrote after coming to live in Devonport.
- Book review “Cured: the life-changing science of spontaneous healing” by Jeffrey Rediger
Cases of the phenomenon variously called “spontaneous healing” or “spontaneous remission” or “remarkable recovery” are sometimes reported in the medical literature, usually in relation to advanced cancer. They are probably not quite so rare as followup statistics suggest, either because sceptical doctors presume that the original diagnosis was wrong, or because the patients concerned have stopped attending hospital clinics. Jeffrey Rediger, a physician and psychiatrist who is on the faculty of Harvard Medical School, has spent fifteen years studying this topic by interviewing patients and visiting healing centres. In his book, case histories are interwoven with summaries of the latest research into the body’s defences against disease.
The library copy of Cured on which I based this review is subtitled “the life-changing science of spontaneous healing” by Jeffrey Rediger but the version on the Amazon page, presumably more recent, has “the power of our immune system and the mind-body connection” by Jeff Rediger. Although I don’t know why the subtitle was changed (or the author’s name shortened) it strikes me that the term “spontaneous” could be misleading. Most unexpected, apparently miraculous, recoveries from a disease that had been considered incurable do not happen out of the blue, but after the patients concerned have taken active steps to reclaim their health.
Early chapters focus mainly on physical aspects, with detailed discussion about how to optimise nutrition, and support the functioning of the immune and nervous systems. The later ones have a more obvious “mind-body” emphasis with topics such as the placebo response, faith healing and prayer, the power of love, and what he calls “healing your identity”.
This last aspect may be of crucial importance. It builds on the work of early researchers such as Lawrence Le Shan, whose book Cancer as a Turning Point influenced my own choice of psycho-oncology as a career, and echoes the message of more recent books such as Remarkable Recovery by Caryle Hirshberg and Marc Barasch. Many of the patients described in these books made a decision, consciously or not, to take control of their lives and “rewrite their stories”. This often involved leaving a toxic relationship or an unsatisfying job, reviving an undeveloped talent or ambition, and most importantly making “deep mental and spiritual changes”. An essential feature was being true to themselves rather than conforming to outside expectations, and following their own path. This might require courage and faith, and the discipline to “burn their boats” to prevent a lapse back to the previous way of life. Some became whole-heartedly committed to particular healing practices. These were very varied, ranging from a strict ketogenic diet to daily immersion in yoga or meditation, suggesting that faith in the chosen modality whatever it may be is the crucial factor in its effectiveness.
This psychological picture does not fit every case. Regression from cancer following an acute infection with high fever is well documented, and must have a biological basis rather than a psycho-spiritual one. Some cases of remarkable recovery do appear spontaneous, because no explanation at all can be found.
Dr Rediger provides plenty of information and guidance for those seeking to prevent disease, or to maximise their chances of recovery from an existing condition, and the case histories are inspiring. He rightly avoids recommending particular approaches, and he acknowledges that there are no guarantees. Plenty of patients “do all the right things” and still succumb to their disease; spontaneous healing remains to some extent a mystery. This is a valuable book, though perhaps rather too long and detailed to be easily digested by someone dealing with a serious illness. Future editions could be made more accessible by adding an index, and summaries at the end of each chapter.
***
Jennifer Barraclough, originally from England and now living in New Zealand, is a retired doctor and a writer of medical and fiction books. A list can be found on her author pages: https://www.amazon.com/Jennifer-Barraclough/e/B001HPXGZI (US) and https://www.amazon.co.uk/Jennifer-Barraclough/e/B001HPXGZI (UK).
- Recovering from wrist fracture: six months on
Six months have passed since I broke my wrist. Having heard from various sources that recovery from this type of fracture should be largely complete by six months, I decided to write what will probably be my last update on the subject, and hope it may be useful for other people dealing with this common injury.
Six months is of course a ballpark figure based on an average of many cases. Healing is a gradual process and its rate varies greatly between individuals. My own recovery is not complete, but there has been a lot of progress. As well as all personal care and household tasks, I can now easily manage the main activities that are important to me: typing on the computer, driving the car and walking the dog. The exception is playing the piano, which continues to hurt. My wrist still looks misshapen and probably always will, but I hope the residual swelling will eventually subside.
At my recent outpatient review with Xray, the consultant orthopaedic surgeon said that the bones were “solidly healed” but that the alignment between radius and ulna was not quite right and therefore certain wrist movements are restricted. He offered an operation to correct the displacement but, considering that this would require another six weeks in plaster with consequent limitation of activity and loss of fitness, I decided not to accept it at present. Surgery can be reconsidered at a later stage, but I hope that my condition will continue to improve on its own.
Finding “silver linings” in an illness is not always easy. I hope this experience has made me more patient, more tolerant of others’ limitations and not in so much of a hurry myself. It has led indirectly to several positive changes: a new choir, a new GP, and attending Pilates and “Silver Swans” ballet classes each week to improve my strength and balance.
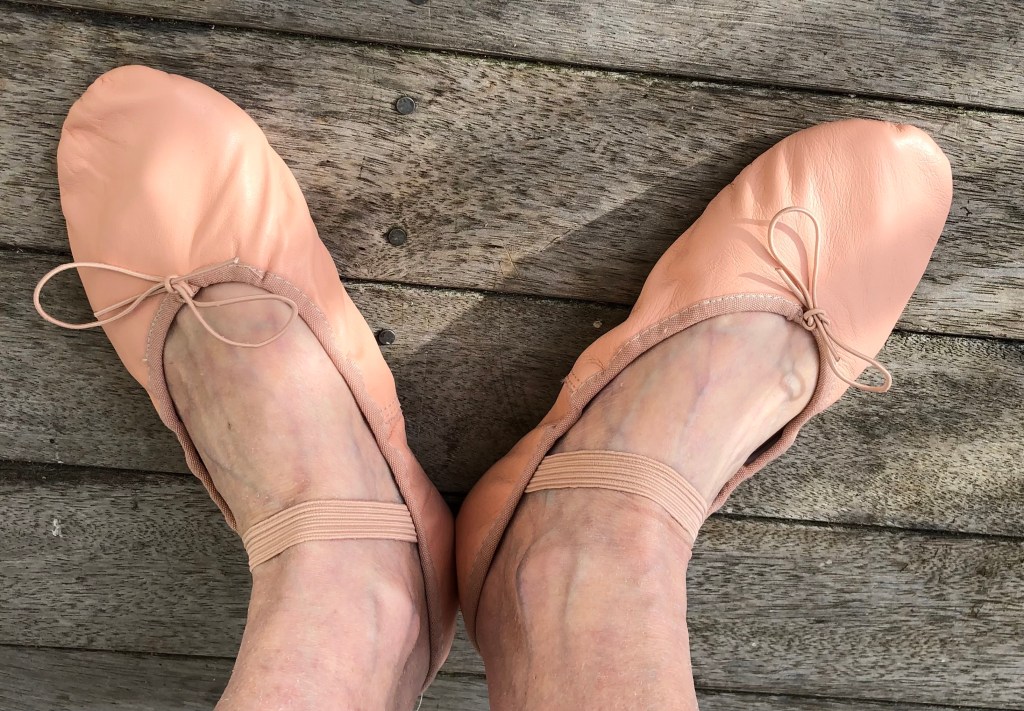
***
Jennifer Barraclough, originally from England and now living in New Zealand, is a retired doctor and a writer of medical and fiction books. A list can be found on her author pages: https://www.amazon.com/Jennifer-Barraclough/e/B001HPXGZI (US) and https://www.amazon.co.uk/Jennifer-Barraclough/e/B001HPXGZI (UK).
- Books I’ve enjoyed #9
Here is a selection of the books, fiction and non-fiction, that I’ve enjoyed in recent months.
Top pick among my favourite genre of English psychological mystery novels is Magpie Lane by Lucy Atkins. This held a special attraction for me because of its evocative descriptions of Oxford, where I lived for many years but have been unable to revisit since the pandemic began. Its unusual protagonist is a Scotswoman, a mathematics dropout who works as a nanny for academic families. She becomes closely attached to her latest charge, an eight year old girl neglected by her self-centred parents. The girl disappears, prompting a police investigation. Another good and original read was The Appeal by Janice Hallett, written mainly in the form of email exchanges among the legal team preparing an appeal against a murder conviction. It is set in a fictional town where the amateur dramatics society includes a large cast of players.
After watching the award-winning film Nomadland, I read the book of the same title on which it was based. The author, Jessica Bruder, is a journalist who spent three years observing and befriending some of the thousands of van dwellers who travel around America supporting themselves with seasonal jobs. The majority are single older people who, though often well qualified and skilled, have met with financial hardship and can no longer afford conventional housing. Their fortitude and ingenuity, as they navigate the practical challenges and endure what sound like appalling working conditions in campsites, Amazon warehouses and beet farms, are impressive. I found this book somewhat long and meandering, but its content was an eye-opener.
The only medical book in this selection is The Sleeping Beauties by neurologist Suzanne O’Sullivan, who has travelled round the world observing “culture-bound” epidemics of illnesses for which no medical explanation can be found. Such syndromes have been described by many different terms including “hysterical” “psychosomatic” and “functional”. The causes may be complex, but the author believes sociocultural factors to be more relevant than than individual psychopathology. I found the discussion sections at the end of each chapter rather heavy going, but I do know how difficult it is to write clearly about this subject. I liked the final section about the growing “over-medicalisation” of life problems in Western countries.
Two autobiographies are on this list. Father Joe: the man who saved my soul is by the late English satirist Tony Hendra, best known for his work on the Spitting Image TV programmes. As a result of a sexual transgression in his teens, he was sent to Quarr Abbey on the Isle of Wight to meet the Benedictine monk who was to become his spiritual mentor throughout his colourful adult life. A very different memoir is One Woman’s War by Eileen Younghusband who, aged nineteen, volunteered to join the Women’s Auxiliary Air Force and worked as a “filterer” transcribing Radar transmissions in WW2. After the war she was posted to Europe and among other duties worked in a liberated concentration camp. This beautifully written short book gives a modest account of an extraordinary life.
I recently wrote a separate post about Happy: why more or less everything is absolutely fine, Derren Brown’s take on Stoic philosophy and other things.
***
Jennifer Barraclough, originally from England and now living in New Zealand, is a retired doctor and a writer of medical and fiction books. A list can be found on her author pages: https://www.amazon.com/Jennifer-Barraclough/e/B001HPXGZI (US) and https://www.amazon.co.uk/Jennifer-Barraclough/e/B001HPXGZI (UK).
- You Yet Shall Die: A psychological mystery about family secrets and a long-ago crime
I’ve recently been so focused on writing my next book that I’ve neglected the marketing of my previous ones. So I’ve now set up a price promotion for the Kindle version of You Yet Shall Die, a gentle psychological mystery set in rural England in the recent past. The novel has 5-star ratings on Amazon, and readers’ comments include “It was superb. Great twist that you didn’t really guess” and “Top marks for an absorbing crime and mystery story without the gory bits.”
How to respond to a stranger who claims to be your half-sister? Hilda, a single woman living as a recluse in a marshland cottage with her rescue cats, is faced with this question when she is visited by a young woman claiming to be the “love child” of her late father. Hilda’s quest to investigate her family background leads to a dangerous conflict with her brother, and to the discovery of some shocking events rooted in postwar Oxford and the 1960s London nightclub scene, but also widens the options for her own future.
The Kindle promotion, available to readers in most but not all countrie, is running from 20-27 June. Please have a look on your local Amazon website, and it would be much appreciated if you can help my marketing efforts by sharing this post with your contacts – thank you.

- Murder mystery in Matakana
Matakana, a pretty village in the wine-growing region north of Auckland, was the venue for Sunday’s launch of the novel Blood on Vines by my friend Madeleine Eskedahl. My husband and I attended the event and stayed in the Matakana Motel overnight.

Matakana Estate, photo from TripAdvisor I am unable to drive while recovering from a wrist fracture, so we took public transport. This involved working out the connections between four bus routes: 814 to Akoranga, NX1 to Hibiscus Coast, 995 to Warkworth and 997 to Matakana. We were almost the only passengers for parts of the journey, and as the modern double-decker NX1 on its dedicated busway sped past the traffic jams on the parallel motorway we wondered why Aucklanders are so wedded to their cars. However the trip did take a long time because the rural buses are infrequent. Our wait in the charming little town of Warkworth was pleasantly occupied with lunch and a riverside walk.
The book launch took place in The Vintry, Matakana, an intimate bar in a complex which also contains a cinema, restaurant and boutique shops. We were served with a selection of local wines accompanied by platters of cheeses and tapas while listening to readings from Madeleine’s novel. I haven’t opened my copy yet so can only quote from the back cover blurb: “… an ex-wine-maker is murdered … a rampage of death is about to rock the local community to its core.” The event was well attended and it was good to see some fellow members of the Auckland Crime Writers group.

Madeleine and Jennifer Afterwards a walk down Wharf Road to the Matakana River. The public toilet buildings at the top of the road looked most distinctive.

Photo by Brian Barraclough A dip in the pool at the Matakana Motel, and a delicious dinner at the Matakana Country Kitchen, rounded off the evening and our overnight accomodation was quiet and comfortable. There was a spot of panic in the morning when, due to a discrepancy between the timetable on the bus shelter and the information on the Auckland Transport app, we risked missing the 997 on its occasional trip from Matakana to Warkworth. But all was well and we were home by lunchtime. It felt good to have had a “mini-break” especially considering that, due to lockdowns, I haven’t been away from Auckland since my last visit to England in 2019.
- Recovering from wrist fracture: ten weeks on
Recovery demands a lot of patience, but there have been several positive changes since my last post five weeks ago. I hope writing these updates will help me to appreciate the progress made, and be useful to readers recovering from similar fractures.
My cast was removed about six weeks after the injury. I was anxious about seeing my wrist again, knowing that the two attempts to reset the displaced bones had been only partly successful and the final position would not be perfect. It did indeed look crooked and thickened compared to the other side, and still does, though I hope some of the swelling will go down in time. It was a relief to have the cast replaced by a removable lightweight splint.
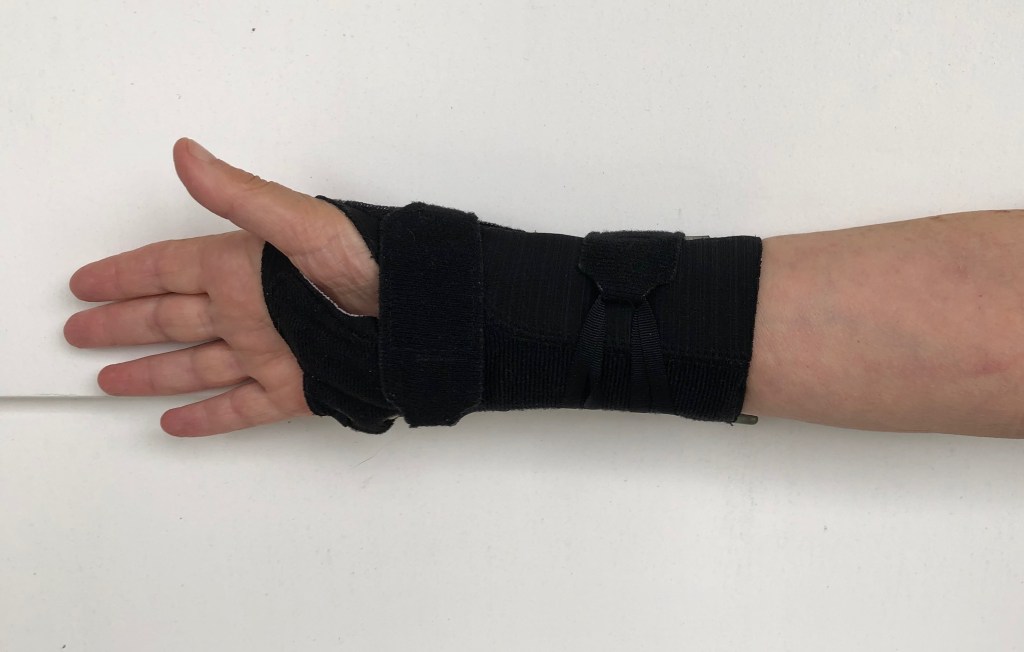
I see a physiotherapist once a week, and carry out the prescribed exercises four times per day. I can’t manage the full range of movements but measurements have shown a slight improvement at each clinic visit. Gently massaging the skin with herbal or homeopathic creams, and essential oils, is comforting. I no longer feel any need to take analgesics, but the ulnar side of the wrist is still stiff and tender, and I understand this can be a persistent problem which might require surgery later on.
As regards daily activities the the most significant advances include being able to drive the car and cut my own nails, though I still can’t use a knife and fork. My general vitality, which was impaired for weeks after the injury, has recovered now and I hope to get back to creative writing soon.
On the negative side, the Dexa scan carried out as part of the follow-up showed reduced bone density. This was disappointing because I take plenty of outdoor exercise and eat the right foods. Before considering medication I shall try extra vitamins and sunbathing, and be more careful about avoiding falls.
All the aftercare is free of charge under New Zealand’s generous Accident Compensation scheme.
- Recovering from wrist fracture: five weeks on
Five weeks have passed since I fell on a rock and fractured my wrist, as described in my previous post Trauma on Cheltenham Beach. Progress has been frustratingly slow, but there are definite improvements. I no longer take painkillers. I have a synthetic cast which is lighter and more comfortable than the plaster one. I can walk the dog using a harness, and fasten my own watch and wash my own hair. I still can’t cut my nails, drive the car, make beds, cope with tight screw tops or plastic packaging. I type and play the piano with one hand.
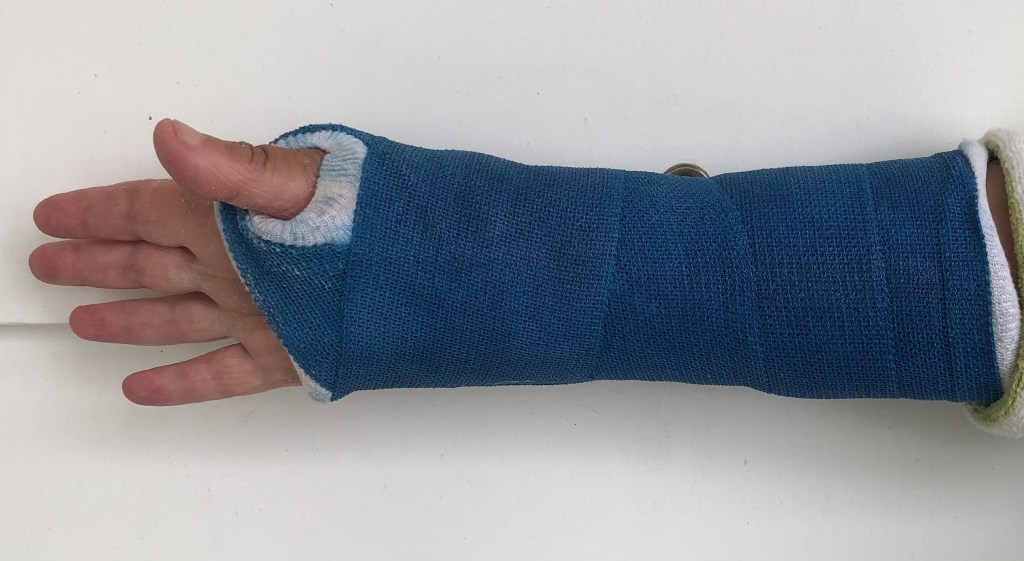
Colles fractures are common. While I am out walking people often ask me what is wrong with my arm, and a surprising number of them have gone on to tell me that they or someone in their family have had a broken wrist themselves. From talking to them I have learned that the outcome can vary a great deal. One woman, who had the same operation that I would probably have had but for the Covid lockdown, reported an excellent result and showed me the barely visible scar. Another had a similar operation which appeared to have worked well until she experienced a return of pain, found to be due to displacement of one of the screws used to secure the metal plate, and is awaiting further treatment. A third, whose fracture was treated conservatively several years ago, has persistent pain and weakness in her wrist. A couple of others, however, have recovered well after conservative treatment. The only man in my little sample, whose injury was very recent, is scheduled for surgery this week.
Clearly the prognosis for each individual depends on details of the fracture and the general health of the patient. There will be many months to wait before I know what it will be like for me.
- Book review “Happy: why more or less everything is absolutely fine” by Derren Brown
My rating: 4 of 5 stars
I have been an admirer of British illusionist Derren Brown since watching his brilliant and controversial TV shows such as “Miracle” and “Sacrifice”. He is also a writer and when I learned that he shared my interest in Stoicism, and that this informed his book Happy: Why more or less everything is absolutely fine, I was keen to read what he had to say. It’s a big book, ambitious and sometimes provocative, spanning a wide range of topics. The style is fluent and engaging, though tends to ramble at times.
I very much enjoyed the potted history of philosophy and psychology, the critical appraisal of the self-help industry, and the practical guidance on modern applications of Stoicism in Parts One and Two. I would have given 5 stars if the book had ended there but was less impressed with Part Three, in which Derren presents his views about death and dying and argues against the existence of an afterlife. Reference to the work of the many thinkers and researchers who have studied these fields, and to others’ contrasting experiences and beliefs, would have made these chapters more balanced and helpful.
Reservations aside, this is an original and stimulating book that can be recommended for serious readers seeking a fulfilling life. - Writing a book is like having a baby
This is a light-hearted piece about the possible parallels between writing a book and having a baby. It’s adapted from Wellbeing for Writers by Jennifer Barraclough, a short guide full of practical tips about finding fulfilment and enjoyment through a writing career.

Although the time it takes to write a book can vary from a few weeks to many years, it is said that the average is about nine months – the same as a full term human pregnancy. But just as some babies are delivered prematurely, some books are submitted for publication too soon, because their writers are so impatient to see them in print. It would have been better to take more time to check for typos in the manuscript and flaws in the plot and generally polish up the finished product. At the other extreme some books, like some babies, become overdue. Maybe the writers are continually revising them in a futile quest for perfection. Or maybe, as first-time authors, they are afraid to take the step of putting their work out to the world.
Of course many pregnancies end in miscarriage. Similarly, many manuscripts are abandoned before they have developed into a complete book. This may not be a bad thing. Writers often need to experiment with different styles, genres and themes and it may become clear that some early drafts are not going to work out well and the best policy is to give up and make a new start.
Just as good care for mothers and babies before the birth is important, writers working on new books need to avoid the physical and mental health hazards associated with their occupation. There’s a chapter in Wellbeing for Writers about how to avoid problems like these.
Publication, like giving birth, is both exciting and stressful. Although writers are spared the physical pain of labor, they may experience acute complications such as discovering a last-minute problem with the proofs, or technical difficulties when uploading their files.
It’s not uncommon for new mothers to develop post-natal depression, due to the huge hormonal and social changes they are experiencing. And writers often feel low after finishing a book, though for different reasons. There is a sense of anticlimax, and sometimes the best treatment is starting to write another one. But inspiration does not come to order, and the equivalent of infertility is writer’s block.
Just as children need care from their parents for many years after they are born, writers need to keep on looking after their books after publication if they hope for ongoing sales, by continuing with marketing and by updating the content if required.
Both having children and writing books represent ways of expressing creativity and leaving a legacy for the future. Just as your children contain some of your genes, your books contain some part of yourself – yet they also have separate lives of their own and you cannot predict or control just how they are going to turn out.
Wellbeing for Writers is available in Kindle or paperback format from your local Amazon website.
- Podcasting
Apologies to those readers who had trouble accessing my site today. I decided to explore the new opportunity from WordPress to create podcasts from my blog posts. With my technical skills being fairly limited, I didn’t manage to record a satisfactory version with my own voice. So I adapted one of my posts slightly so that it would make sense when converted from text to audio and read by “Remy”. I think she reads it very well, even though her American accent may sound incongruous to people who know me! So here is my first podcast, on the topic of “The Fascination of Crime Fiction” – I hope it works.
- Trauma on Cheltenham beach

One of the loveliest walks on Auckland’s north shore, only possible at low tide, goes around the headland between Cheltenham and Narrow Neck beaches. Three weeks ago I set out on this walk but slipped over backwards on a wet rock and automatically put out my hand to break my fall. A sharp pain, accompanied by faintness and nausea, told me I had broken my wrist. A kind passerby helped me walk to the road, and a kind friend drove me to an emergency clinic where Xray confirmed a displaced Colles fracture of the radius and fractured tip of the ulna. Over to the public hospital, and a long wait to have the fracture reduced under local anaesthetic. Home at midnight with swollen fingers peeping out from a pink plaster cast.

Having had previous injuries that recovered quite easily, I wasn’t prepared for the long haul ahead. For the first fortnight I was constantly in pain, and struggled with basic self-care. It was a great help to have my husband taking over household tasks, and relatives and friends providing meals. I expected the worst would soon be over, but met with a setback. A followup Xray at the outpatient clinic showed that the bones had slipped back out of place and a further attempt at reduction, this time without local anaesthetic, was unsuccessful.
Surgery was proposed. I packed my bags and spent an anxious few days awaiting the call to come into the hospital, after starving from midnight. But apparently, discussion within the orthopaedic team had reached the conclusion that the likely benefit of the operation was too marginal to justify the risks (and New Zealand had just gone back into another Covid lockdown, limiting hospital services). I’ll find out more at my next appointment this week, but from what I gather so far the recovery will be a slow process and I’m likely to be left with some permanent deformity and weakness. Things could be far worse, I know, and I hope to be able to return to my former activities of dog-walking, cathedral choir, swimming and driving before too long. Meanwhile I can still go for walks, and enjoy the glorious summer weather. And in theory I have plenty of time to work on my next novel, though typing with one hand is cumbersome and inspiration lacking.
I’d like to be able to say that my recent exploration of Stoic philosophy is helping me to cope with all this. A recent article https://classicalwisdom.com/philosophy/stoicism/marcus-aurelius-stoicism-and-pain/ emphasises the basic precept of focusing only on those aspects of an illness or injury that are under personal control – for example making informed choices about treatment, and taking general steps to maintain a healthy lifestyle. There is no point dwelling on the negative aspects, or getting stuck in feelings of resentment, frustration or regret. The aim is to accept the situation and develop a constructive response. Simple basic advice, not so easy to put into practice.
***
Jennifer Barraclough, originally from England and now living in New Zealand, is a retired doctor and a writer of medical and fiction books. Details can be found on her author pages: https://www.amazon.com/Jennifer-Barraclough/e/B001HPXGZI (US) and https://www.amazon.co.uk/Jennifer-Barraclough/e/B001HPXGZI (UK).
- Summerland and Hope Gap
For many years after coming to live in New Zealand in 2000, I was able to make regular return visits to England to see my friends, relatives and favourite places. Spending a day with Lesley, who lives in East Sussex, was a regular feature. After having lunch either at her home or in a local pub we would go for a walk on the windswept downland between Seaford and Eastbourne with its views of the Seven Sisters cliffs (inspiring a scene in my novel You Yet Shall Die) followed by a cup of tea in her beach hut.

My 2020 visit had to be cancelled due to the pandemic restrictions. It’s been some compensation to be able to talk to people on Zoom, and to see my home country on screen. I was excited when Lesley told me that two movies – Hope Gap and Summerland – had been filmed in the area where we used to walk.
Hope Gap, which I saw last year, is a family drama charting the breakdown of the marriage of a middle aged middle class couple. Their young adult son takes long walks by the sea while pondering how to mediate between his introverted father, who has announced that he is leaving to live with another woman, and his melodramatic mother who is devastated by the situation. This film tackles its subject seriously but with touches of humour. It would not be to everyone’s taste, but I found it an absorbing story intelligently told.
Summerland has only just arrived in New Zealand cinemas and I saw it yesterday. The main action is set during World War 2. A reclusive woman writer, embittered since the ending of a lesbian love affair, is furious when she is forced to take in a boy evacuated from bomb-ravaged London. Predictably, her heart eventually softens and the film has a happy ending. I found the story rather sentimental and contrived, but the scenery was lovely. Although allegedly taking place in Kent, most of it had been filmed in the same part of the East Sussex coast pictured above.
***
Jennifer Barraclough, originally from England and now living in New Zealand, is a retired doctor and a writer of medical and fiction books. A list can be found on her author pages: https://www.amazon.com/Jennifer-Barraclough/e/B001HPXGZI (US) and https://www.amazon.co.uk/Jennifer-Barraclough/e/B001HPXGZI (UK).
- Stoic perspectives on death and bereavement
New Year’s Eve 2020 was the fifth anniversary of my mother’s death. I have finally destroyed her personal papers (see my earlier post) but the memories, both happy and sad, remain. Many other relatives and friends of my husband and myself have also died in recent years, and we are getting old ourselves. I had a lot of professional exposure to death and bereavement during my medical career, but the personal experience is very different. I’ve been exploring what the ancient Stoic philosophers had to say about this subject, hoping it may prove helpful for coping in future. The Stoics believed in facing up to death as a natural process which is nothing to be afraid of.
A central tenet of Stoicism is that only our own judgments and voluntary actions are “up to us”. Other aspects of life are not, and although some of these “externals” are to be preferred over others, they are best regarded with indifference. Death, an external that is inevitable for all living things, is only bad if we consider it to be so and sometimes may be welcome.
Epictetus: Death is a release from and an end of all pains: beyond it our sufferings cannot extend: it restores us to the peaceful rest in which we lay before we were born.
The Stoics believed that the timing and manner of death, random and cruel as it may seem, is determined by fate and not up to us. This is less true now that advances in medical science have enabled more control over health and longevity than was available to the ancient Greeks and Romans, but much unpredictability remains. We and those close to us are all going to die one day – maybe tomorrow. Frequent contemplation of this prospect (the Stoic practice of memento mori), is not intended to promote morbid obsession, but to emphasise the importance of making the most of the “festival of life” every day, not wasting time, and appreciating our loved ones while they are still here.
When a loved one dies there will inevitably be distressing reactions such as shock, grief and anger. While negative emotions in the short term are natural, the Stoics advised aiming to move on as soon as possible towards a calm acceptance of the person’s death; continuing to remember them often, but with love and appreciation rather than with sorrow.
Seneca: Thinking of departed friends is to me something sweet and mellow. For when I had them with me it was with the feeling that I was going to lose them, and now that I have lost them I keep the feeling that I have them with me still.
This approach will appeal to some people, while striking others as unrealistic or heartless. It is rather different from today’s prevailing view of mourning as a gradual process of working through the “stages of grief” over many months, perhaps with the aid of bereavement counselling. Everyone is different, and the best way of coping depends on individual personality and circumstances. One idea I have found helpful myself is to think of the deceased as having been “reclaimed by nature”, as all living things will be one day, rather than “lost”.
Epictetus: Is your child dead? It has been given back. Is your wife dead? She has been returned.
What about the soul or spirit, and the question of an afterlife? As I understand it the Stoics believed that death is probably followed by the same oblivion that existed before birth, and that individual immortality is unlikely.
Marcus Aurelius: Just as on earth, with the passage of time, decaying and transmogrified corpses make way for the newly dead, so souls released into the heavens, after a season of flight, begin to break up, burn, and be absorbed back into the womb of reason, leaving room for souls just beginning to fly. This is the answer for those who believe that souls survive death.
***
Jennifer Barraclough, originally from England and now living in New Zealand, is a retired doctor and a writer of medical and fiction books. A list can be found on her author pages: https://www.amazon.com/Jennifer-Barraclough/e/B001HPXGZI (US) and https://www.amazon.co.uk/Jennifer-Barraclough/e/B001HPXGZI (UK).
- Changing choirs
Twenty years ago I joined the alto section of the choir of St Patrick’s Cathedral in Auckland. My previous musical experience had been rather limited – as a child I reluctantly attended some piano lessons, and as a student I sang in the chorus of The Pirates of Penzance. But in 2001 the cathedral choir was open to anybody who wanted to join, no audition required. There were about 30 members. It was all new to me but I sat next to an experienced singer, Marion, who took me under her wing and has remained a close friend ever since.
I loved singing the sacred music, including well-known classics such as Mozart’s Ave Verum Corpus and Franck’s Panis Angelicus, Renaissance motets by composers such as Tallis and Palestrina, and occasionally more modern works such as John Rutter’s Magnificat. I bought a piano, took some more lessons and did well in a theory exam although my practical skills hardly improved.
Apart from the beauty of the music, a benefit of belonging to the choir was meeting people of all ages and a wide range of nationalities including Filipino, Samoan, Korean, Chinese, American, French as well as both Maori and Pakeha native New Zealanders. I was usually the only English person there.
Over the years there were many changes. Old members left, new ones joined, and we had a series of musical directors each with their own different methods. The trend has been towards a smaller group with stricter technical standards.
Belonging to the choir was a wonderful experience but couldn’t last for ever. Others had retired when they turned 70 – I stayed till 74, but was starting to find it arduous. The rehearsals and services were longer than in the old days, transport from home was more frequently delayed, and decreasing stamina made it harder to cope with the physical demands. After breaking my wrist recently I had to take two months off anyway, and then I made the hard decision not to go back. Leaving felt sad, and still does, though I do appreciate having extra free time on Sunday mornings.
I wanted to continue some singing, because I enjoy it very much and it has many proven benefits – physiological, intellectual, emotional, spiritual and social. So I have now joined a women’s community choir, which is more local, and involves attendance only once a week instead of twice. The atmosphere is relaxed and friendly, but some of the music is quite challenging, with songs in various styles from around the world forming quite a contrast to the repertoire at St Patrick’s.
- Books I’ve enjoyed #8
Continuing my bi-annual list of book recommendations, here’s a selection from my reading list of recent months.
Literary fiction: I presume it’s just coincidence that the two novels I’ve enjoyed the most are both about inhibited older Englishmen with links to former British colonies. Old Filth by Jane Gardam, in which an old judge takes stock of his complex past life, is a masterpiece. The Mission House by Carys Davies, a much shorter book, is an elegantly written story about a depressed librarian’s sojourn in the hills of India.
Stoic philosophy: Though I have yet to tackle any of the ancient texts, a recent interest in this topic has led me to read several modern ones. Lessons in Stoicism by John Sellars gives an excellent short introduction. I have also enjoyed books by Donald Robertson, William Irvine and Massimo Pigliucci. Next year I intend to work through The Daily Stoic Book by Ryan Holiday and Stephen Hanselman.
Psychological thrillers: I read a lot of novels in this genre, and here are three of the ones I’ve enjoyed most. I was interested in Stone Mothers by Erin Kelly because it is set in an old county mental asylum similar to those where I worked many years ago. Here to Stay by Mark Edwards is a gripping account of an in-laws’ visit which goes from bad to worse. Who Did You Tell by Lesley Kara is about a young woman in a seaside town struggling to maintain sobriety and come to terms with an event from her past.
Biography and memoir: A Bit of a Stretch, the diary kept by Chris Atkins during his spell in a London prison, describes the appalling conditions in a darkly humorous style. Unorthodox by Deborah Feldman, the book on which a recent Netflix hit was based, is about her repressed upbringing in an ultra-orthodox Jewish community in New York. On Chapel Sands by Laura Cumming, set on the Lincolnshire coast, describes a different kind of unhappy childhood in gentle prose.
From my large pile of other books waiting to be read over the Christmas and New Year holidays, I’ve just started reading How to Walk a Dog by Mike White; a collection of entertaining though sometimes poignant true stories about the human-canine bond.
***
Jennifer Barraclough, originally from England and now living in New Zealand, is a retired doctor and a writer of medical and fiction books. A list can be found on her author pages: https://www.amazon.com/Jennifer-Barraclough/e/B001HPXGZI (US) and https://www.amazon.co.uk/Jennifer-Barraclough/e/B001HPXGZI (UK).

Photo by Pixabay on Pexels.com - “Wellbeing for Writers” revisited
Five years ago I wrote a short ebook called Wellbeing for Writers, based on my experience of having writers as clients in my life coaching and Bach flower practice, and on the rewards and challenges of my own writing career. It contains practical tips about technical and commercial aspects for those new to the field, but is mainly focused on psychological ones that may also be relevant for experienced authors. Why do you write, and is it primarily for yourself or for your readers? How to protect time for writing when working from home with family responsibilities? How to respond to rejection and criticism? How to overcome a phobia of marketing? How to avoid the physical and mental health problems that particularly affect writers? What personal qualities and values are relevant to fulfilment and success?

Wellbeing for Writers had sales and positive reviews to begin with, but then lapsed into obscurity like so many of the other books on Amazon (according to one unofficial estimate, there are over 48 million of them now). I had more or less forgotten about it myself until an email inquiry prompted me to read it again and make a few updates.
Revising an older book can be a rather tedious task and is often neglected, though with non-fiction topics for which new knowledge and information frequently become available, it really ought to be done every few years. The content of Wellbeing for Writers required little change apart from a few corrections. Some of the website links had become invalid and, to my embarrassment, I found that Virginia Woolf’s name had been wrongly spelled in the original version.
Wellbeing for Writers by Jennifer Barraclough, ASIN B00YWEK97Y, is available from your local Amazon store in Kindle format (if you don’t have a Kindle you can read it with the Kindle App on another device).
- Stoicism for writers and healers
I’ve been reading some basic books about Stoic philosophy, which originated in Ancient Greece and Rome, and describes a path to a good and happy life lived in harmony with others and with nature. It has much in common with other systems and many of the ideas were already familiar to me from Buddhism, Christianity and modern psychological therapies, but it is refreshing to have them presented in clear practical terms. Here are a few thoughts from a novice student of Stoicism.
One of the principles stated by Epictetus (50-135 AD) resonates strongly with me. He wrote that “some things are up to us and some things are not up to us”, so it follows that we are well advised to focus only on what is within our control – which includes very little except our own judgements and behaviours. This may sound simple and obvious (and the “serenity prayer” of St Francis, which I have heard so many times, says something similar) and yet I am certainly not alone in having wasted much futile effort and distress over things which I have no power to change. Applying this principle would avoid many of the hassles of daily life, such as frustration in a traffic jam or irritation with an untidy workmate. It is also relevant to both the two fields – writing and medicine – in which I have spent my career.
As a writer it is up to me to make my books “the best they can be”, to choose whether to submit them to traditional publishers or to publish independently, and decide how much time and money to spend on marketing. But whether people want to buy my books, and whether readers like them, is not up to me. So there is no point in getting upset over rejection letters, lack of sales or negative reviews – in theory. In practice, overcoming the desire for external validation and becoming more tolerant of criticism requires mental discipline and training.
Turning to the medical field, again there is a dichotomy between what is “up to us” and what is not in relation to physical health. We can make choices about many aspects of our lifestyle and behaviour, such as diet and exercise, in the hope of preventing or recovering from disease. But there is no guarantee that our efforts will be successful, and nor can we change some of the other factors such as our genetic susceptibilities, exposure to pathogens in the environment, the inevitable deterioration of our bodies as they age. The dichotomy between what we can or cannot control is not always acknowledged. Some put all their faith in external treatments with drugs and surgery, and ignore what patients can do to help themselves. Others advocate total personal responsibility for health, and risk making patients feel guilty for being ill. Both extremes are potentially dangerous.
There is of course much more to Stoic philosophy than this and, having enrolled in the annual online event Stoic Week which is about to start, perhaps I will write more blog post(s) on this subject.
- Why I still admire Agatha Christie
I loved Agatha Christie’s books when I was a teenager. I read most if not all of her 66 crime novels featuring the detective skills of Hercule Poirot or Miss Marple, and occasionally other characters such as Ariadne Oliver or Tommy and Tuppence. Many years later I still have a few dogeared paperback versions, passed down from my mother’s estate, and look at them occasionally.
Agatha Christie’s writing career spanned more than 50 years, from 1920 to 1974. The majority of her books are set between the two world wars, a period that has been called the Golden Age of detective fiction. They seem old-fashioned today, yet I still find them appealing, and am obviously not alone in this. Her novels are still widely read, and new dramatisations and pastiches of her work and biographies of her life continue to be produced.
What is the secret of their enduring popularity? For me, there are several reasons:
The plots, mostly following a classic “whodunnit” formula, are extremely ingenious. Although there are clues scattered throughout the books, the solutions cannot easily be guessed before the end. It is said that the author herself often did not know the identity of the murderer until she had written the first draft, which seems amazing if it is true.
The books provide an authentic picture of an England that no longer exists – a time when life was simpler and more slowly paced, comfortable middle class families in quaint villages or country houses were supported by domestic servants who knew their place, and male and female roles were clearly defined. Whether you feel some sense of nostalgia for those days, or are thankful they are gone, it is interesting to read about a relatively recent period of English history so different from today.
Agatha Christie’s style is highly readable. She had a remarkable gift for writing with a light and sometimes humorous touch, but without trivialising the serious subject of murder. Her characters, if somewhat stereotyped, are mostly sympathetic. There is no graphic sex or violence in her books, and they are often categorised today as belonging to the “cozy crime” genre – a term which seems to me to devalue them. They are quite short, I think around 60,000 words. Many modern crime novels are twice that length, but personally I find the more concise format more satisfying.
As you can see from its cover image, there are references to Agatha Christie’s work in my own recent novel You Yet Shall Die. Set in rural England between the 1950s and early 2000s, it is a story of family secrets and discovery of a long-ago crime. If you haven’t had a chance yet, please have a look on Amazon.com or Amazon.co.uk.

- “Beautiful Vibrations”: Living through medical illness with Bach flower remedies

Dr Edward Bach described his flower remedies as having “beautiful vibrations” capable of promoting positive mental states such as hope, courage and calm. Established as a safe and natural therapy for almost 100 years, they can help to relieve the emotional distress often associated with physical illness. This short practical guide explains how to select and use the remedies as part of a holistic approach to healing. There are sections on common problems such as anxiety and sadness about the medical condition and its treatment, and difficulty in adjusting to changes in lifestyle and relationships. Despite all its negative aspects, serious illness can have “silver linings” and the flower remedies can help to bring these out.
Dr Jennifer Barraclough is a former consultant in psychological medicine with many years’ experience of working with patients and their families especially in cancer care settings. She is also a qualified Bach flower practitioner, life coach, and author of fiction and nonfiction books.
Beautiful Vibrations is available from your local Amazon website:
Amazon AU: Kindle
- Author profile pictures
During the interval between lockdowns I decided to have some professional portrait photos taken, for use on my website and elsewhere. I was quite nervous before my session at headshotstudio.co.nz in central Auckland, but the afternoon with photographer Richard and makeup artist Ruth turned out a very enjoyable experience.
I had previously been using some amateur photos on my social media. The snaps of me holding cats or kittens were nice but maybe too informal. I rather liked another which showed me drinking wine at a cafe but perhaps this gave the wrong impression.
Like book covers, which I wrote about in my last post, author photos are a marketing tool which should ideally convey an impression appropriate for their genre. A crime writer might want to look slightly sinister or mysterious, a romance writer attractive and glamorous, a writer of medical books serious and academic. When I read a book I always hope to see a photo in the About the Author section at the back, though sometimes there isn’t one.
As I have written in several different genres myself, I aimed for nothing more specific than having a nice picture taken before the ravages of time affect my appearance any more than they have already. Here are the two of the best ones from my recent shoot.


- Changing covers
As a self-published author I really enjoy choosing the covers for my books, but have learned that it’s not just about finding a pretty picture. The cover image is very important for marketing purposes, so it can be worth employing a professional designer rather than relying on stock photos. “Don’t judge a book by its cover” may be good advice in theory but, in practice, our first impressions about both objects and people are usually based on their appearance. A split-second glance at the cover often determines whether or not a potential reader will look inside.
What makes a good cover for a novel? Ideally the image, in combination with the title, will “capture the essence of the book” so as to appeal to its target audience – a tall order. Experts advise that the image should be relevant to the genre, but distinctive enough to stand out from other titles in the field. It should convey something about the story in a way that excites readers’ curiosity. The design is best kept fairly simple, with a single focal point to draw the eye, and needs to look good in thumbnail view. Personally I think the colour scheme is also very important.
A highly skilled artist may be able to ignore these rules, and create a cover image which looks so stunning that it attracts potential readers even if it bears no obvious relation to what the book is about.
Revamping a book’s cover from time to time can stimulate sales by attracting a fresh group of readers, and I recently changed the image for my novel You Yet Shall Die. The original version showed a photo of the North Kent marshes, where much of the story is set. I really liked the appearance of that one, but it gave little indication of the genre or content. The new version, featuring an old-fashioned dressing table strewn with books, is more relevant to the plot and more likely to appeal to the mature women who are the main target audience – hopefully without putting off all the men, considering that several of my male friends have enjoyed it.


Original cover on the left, new one on the right.
You Yet Shall Die is a gentle mystery novel set in Kent and Sussex. Who is the woman who claims to be Dr Harper’s “love child”? What was the true cause of his wife’s early death? As Hilda Harper researches her parents’ early lives in postwar Oxford and Swinging London’s nightclub scene, she discovers some shocking secrets but also finds new hope for her own future. You Yet Shall Die is available in paperback or ebook format from Amazon.com, Amazon.co.uk and other Amazon marketplaces.
- Books I’ve enjoyed #7

Photo by Anna Shvets on Pexels.com A positive aspect of my lockdown experience was having more time to read, which enabled me to finish a very long book – The Mirror and the Light by Hilary Mantel. This is the final volume of her Thomas Cromwell trilogy set in England during the reign of Henry VIII, the first two books in the series being Wolf Hall and Bring up the Bodies. Although I would have enjoyed it even more if it had not been quite so detailed, the trilogy – a product of extensive historical research and vivid imagination – is a monumental achievement.
Another “faction” book (that is, a book based on a historical figure or events interwoven with fictitious elements) is The Surgeon of Crowthorne by Simon Winchester. The surgeon in question, WC Minor, murdered a man under the influence of paranoid delusions and was committed to Broadmoor Hospital in 1872. During the long years of his confinement there he devoted himself to researching the origin of words, contributing over 12,000 quotations to the first edition of the Oxford English Dictionary. This book was recently made into a film called The Professor and the Madman.
Having spent my professional life in general hospital psychiatry I am interested in popular books based on real-life case histories. Writers in this genre face a challenge; they must alter the details enough to preserve patients’ confidentiality, but not so much as to sacrifice medical accuracy. Three such books I have read this year are Love’s Executioner by Irvin Yalom, an American psychotherapist; Into the Abyss by Anthony David, a British neuropsychiatrist; and The Prison Doctor by Amanda Brown, a British GP.
I enjoyed autobiographies by two very different women. Lady in Waiting by Anne Glenconner is an engaging description of the life of a socialite who was born and married into the British aristocracy and had close connections to royalty, especially Princess Margaret. Her family’s privileged and hedonistic lifestyle was no protection against a series of tragedies, and after reading this book I felt glad that my own social background was more ordinary. Becoming by Michelle Obama is a longer book written in a more serious style. Born into a modest, hardworking black family in Chicago, she qualified as a lawyer and could have pursued a high-flying corporate career, but elected to focus instead on community and social issues, and as the wife of Barack Obama spent the years 2009-17 as First Lady of the United States.
***
Jennifer Barraclough is a retired doctor, originally from England but now living in New Zealand, who writes medical and fiction books. Her latest novel You Yet Shall Die is a mystery about family secrets and a long-ago crime.
- Older books: renounce or revive?
Today I donated the last box of my book Focus on Healing to the church fair. It was published just before print-on-demand paperbacks and ebooks became widespread, and although it was well received by readers, more copies were printed than were sold. I didn’t want to be like the author I once heard about whose garage was full of his own books when he died, and whose heirs gave the books away at his funeral.
Just as new cars start losing value as soon as they are sold, books on medical and healthcare topics start going out of date as soon as they are published. The content of Focus on Healing is still valid, and the ebook version is still available, but there is new information that could be added if I wrote a second edition. I’m not intending to do that, because I no longer work in the healthcare field.
Novels do not go out of date in the same way, although most sales usually occur in the first few months after publication. My own latest You Yet Shall Die is certainly selling better than my earlier ones, the Dr Peabody series which provide a somewhat cynical picture of medical practice in the 1980s, and the Three Novellas which are mystery/romances set between England and New Zealand. Some readers dislike older novels simply because their content seems out of fashion, or because they convey racist or sexist views, intolerance of minority groups, or other attitudes that would be indefensible today. Other readers accept these things as representative of the time the novels were written, and find that the historical aspect adds to the interest of the story.
A few older books become classics. Most of them fade into obscurity unless, rather sadly I think, they only become popular after being mentioned in the author’s obituary.
For details on the books mentioned here, please visit my Amazon author page.

- Expat blues
Even though I’ve been very happy living in New Zealand for the past twenty years, I expect England will always feel like home. I’ve been fortunate to be able to return for a short visit every summer – until now. I had booked to fly to London next week but my trip has been cancelled due to Covid-related restrictions.
Earlier visits involved a joyful, if exhausting, whirlwind of activity – travelling round the British Isles by train and plane, staying a night or two in several different places, often having lunch, tea and dinner engagements with different people on the same day. The itinerary has gradually become less demanding, as I realise I can’t see everyone every time, so recently I’ve just stayed in London and done day trips. I always try to see my closest friends and relatives, and visit some favourite places – Oxford, Malvern, the countryside of Kent and Sussex – which hold special memories or are featured in my novels. I also like to visit one or two tourist attractions such as Blenheim Palace or the Tower of London. And I always buy something from Marks and Spencer.
The change to a less hectic pace is partly my own choice, as I don’t have so much energy as I used to, but partly because my circle of friends – mostly in their 70s and 80s – is shrinking. Six of those I knew and loved have died in recent years. I was able to visit all of them in the last months of their lives, but because of being back in New Zealand was unable to attend any of their funerals. Several of my surviving friends are unwell at present, and one of the hardest things about being unable to travel this year is not knowing when and if I will see them again.
Apart from that, I don’t mind staying home. I have my memories and photos of England, and the internet has made it easy to keep in contact with people at the other side of the world, even if not all of them can accesss Zoom. I’m glad not to be parted from Brian, the cats and the dog. And Auckland is a lovely place to be, even in winter, with the weather reasonably warm and many flowers in bloom.
***
Jennifer Barraclough’s latest novel You Yet Shall Die, set in Kent and Sussex, is available from Amazon.


- Memories of a childhood in Kent

Apple blossom in Kent: photo courtesy of Bruce Williamson on Unsplash Until the age of nine I lived with my family in Gravesend, Kent. I was happy there and did not want to leave, but life took me in other directions and it was about sixty years before I went back. I found many changes, but still felt an attachment to the town and the surrounding countryside, and had intended to return this summer from my present home in New Zealand. That trip is no longer possible because of coronavirus travel restrictions. Instead I joined several Facebook groups devoted to the area, and seeing all the old photos posted there has triggered a few memories of my own.
Our address was 22 The Overcliff, a Victorian house which is now a children’s day care centre. I believe there had been an orchard on that site, and the back garden contained many fruit trees, mainly apples and pears. The Bramley apples, individually wrapped, were stored in the basement over the winter. The front bedroom looked out over the Thames, with the port of Tilbury on the other side, always busy with ships sailing in and out. Between the street and the river was a disused chalk quarry where I used to play, for children were left to their own devices in those days. It was a short walk down to the river itself, and it was there that I learned to swim; no doubt the waters were polluted but I came to no harm.
I attended Milton Road Primary School but remember very little about that, and it’s not there any more. My best friend was called Jennifer Clements; we lost touch years ago.
Much clearer memories relate to outings with my grandfather, Ernest Guy. He was head of the Technical School in the 1940s till the early 50s. He had a great love and knowledge of the English countryside and, especially after he retired, took every opportunity to drive his old black car (an Austin 7?) to different parts of Kent. Summer holidays were spent camping in the Isle of Sheppey, or visiting resorts on the south coast.
Short local visits involved identifying wild flowers and birds, exploring local churches, collecting nuts or blackberries or mushrooms to cook for tea. I remember the orchards and hop fields and oast houses, and walks near Meopham, Shorne, Cobham Woods, Holly Hill … and wonder how many of the old footpaths and woodlands have now been built over, and how many “areas of natural beauty” developed into tourist sites. With no prospect of international travel in the near future perhaps it is best to remember these places as they used to be.
***
Jennifer Barraclough is a retired doctor, originally from England but now living in New Zealand, who writes medical and fiction books. Her latest novel You Yet Shall Die, a family mystery set on the North Kent marshes, is available from Amazon.com.
- Letters from the past
Over four years have passed since my mother died. The financial side of her estate has finally been settled, following prolonged correspondence with accountants and lawyers. A personal aspect, namely the letters in two of the box files I discovered in the spare bedroom when clearing her house, remains unresolved. I hope this is the last weekend of the Covid-19 lockdown, which would seem an ideal opportunity to deal with these boxes before my life gets busy again. But I still can’t decide what to do with them.
One box contains a series of letters written to my mother during my childhood in the 1950s and 60s, regarding a situation of which I was only dimly aware. I don’t know whether she intended me to find them after her death, but as she was a very “private person” I suspect not. I did read them, while feeling somewhat guilty about doing so. I think it likely that she intended to destroy them one day, but having become weak and unwell in the last months of her life, either lacked the energy to do so or forgot they were there. I haven’t shown the letters to my husband, but he knows something about their content, and suggests that it could make a good basis for my next novel. This may be true, but writing such a book would seem disloyal however heavily I disguised the plot. I have several options. I could destroy all the letters now. I could go through them again and copy selected extracts into a file on my computer for future reference, then destroy the rest. I could leave them in the box, with a note asking whoever finds them after my death to destroy them unread.
The other box contains the letters I sent home to my mother and grandparents in Yorkshire when I was a medical student in Oxford in the late 1960s. I have only reread some of these, having found the style embarrassingly naive, but some contain descriptions of the course which might perhaps be of interest to a medical historian. I was shocked to find that I remember nothing about most of the people and events described. What a contrast to my husband Brian Barraclough and my friend Jean Hendy-Harris, who can both recall their past lives in great detail and have published memoirs about them. I wonder which of us is the more unusual.
Update December 15 2020: With the fifth anniversary of my mother’s death approaching, it was time to make decision about her letters. I destroyed them all yesterday, not without regret, but felt it was the right thing to do.
***
Jennifer Barraclough is a retired doctor, originally from England but now living in New Zealand, who writes medical and fiction books. Her latest one You Yet Shall Die, a novel about family secrets and a long-ago crime set in southern England, is available from Amazon and other online retailers, or can be ordered from bookshops and libraries.
- A psychiatrist remembers
Many friends and former colleagues of my husband Brian are already reading A Partly Anglicised Kiwi: a psychiatrist remembers, the newly published memoir about the first 32 years of his life. The main focus is on Brian’s experience of the psychiatric training programme at London’s Maudsley Hospital in the 1960s. There are shorter sections on miscellaneous topics such as being a patient in a TB ward, and tramping in the southern alps of New Zealand.

To quote from Brian’s Introduction:
“In 1962, aged 28, I left my home in New Zealand and sailed to England as a ship’s surgeon. I was on my way to apply for the world’s foremost training programme in psychiatry at the Maudsley Hospital in London.
“Part I of my memoir describes growing up in Auckland, studying at Otago University Medical School, and practising as a doctor in New Zealand. Part II is about my three years at the Maudsley, where I worked in general psychiatry and some subspecialties. Given my modest beginnings, the intellectual and cultural life of London came as a revelation. I received a liberal education from my peers, took holidays in Europe, had a psychoanalysis, and a bad trip with LSD.”
The book was mainly compiled from the essays Brian has written over the years, originally for his own satisfaction rather than intended for publication. My role as editor was to arrange them in a logical order, check for consistency of style and grammar, and discuss with Brian how much material needed to be removed as potentially offensive or libellous. In my experience, writing or editing books is easier done alone than in collaboration with others, and we didn’t always agree. However we are both happy with the finished product, and hope readers will enjoy it.
A Partly Anglicised Kiwi (ISBN 9798623114792) can be purchased from Amazon websites including Amazon.com, Amazon.co.uk and Amazon.com.au. Shipping restrictions at the time of writing may prevent readers in some countries from buying the paperback version, but the Kindle ebook is available worldwide.
***
Jennifer Barraclough is a retired doctor, originally from England but now living in New Zealand, who writes medical and fiction books. Her latest one You Yet Shall Die, a novel about family secrets and a long-ago crime set in southern England, is available from Amazon.com, Amazon.co.uk, Smashwords.com and other online retailers, or can be ordered from bookshops and libraries.
- Writing in lockdown
For the sake of all the people round the world who are suffering real hardship linked directly or indirectly to Covid-19, I do hope the epidemic will soon be over and the lockdowns can be eased. For myself the restrictions have caused nothing worse than frustration, and as far as writing goes they have had their positive side. No longer able to have coffee with friends, go to the cinema, sing with my choir, do my own shopping or volunteer at the SPCA, I am largely confined to house and garden. Domestic work is only satisfying to some extent, and Netflix only enjoyable for limited periods. The highlight of the day is the afternoon walk with Ireland, my dog-share Labrador, but there is plenty of free time.

Ireland ready to go home after his walk
Having this time has motivated me to resume two writing projects that had been flagging lately. On a friend’s recommendation I downloaded the Scrivener programme and am very glad I did so. To learn to use the system I needed some documents to work on, so was stimulated to make a start on the new novel for which vague ideas had been floating round in my mind for some time. I am not the sort of writer who can summarise the whole structure of a book in advance, and work through the chapters in sequence from beginning to end. For a novel I tend to start with a general sense of the theme, setting and characters, writing fragments as they occur to me, before putting them together to form an outline of the plot, which will probably change when I fill it out in more detail. Scrivener, using templates for both fiction and non-fiction, is ideally suited for this way of writing because it enables everything – draft chapters with notes and summaries, character sketches, links to relevant websites and images – to be seen at a glance and arranged in any sequence.
My other project has been the editing of my husband’s memoir about the early years of his life, 1933-65, mainly focused on his psychiatric training at the Maudsley Hospital in London. Collaborating with each other on this book has been a long process, sometimes fraught. However we both agreed on the final version, which will be published shortly – details in my next blog post. The book may appeal to those with an interest in medical history, and to anyone who knows Brian or used to work with him.
***
Jennifer Barraclough is a retired doctor, originally from England but now living in New Zealand, who writes medical and fiction books. Her latest novel You Yet Shall Die is available from Amazon.com, Amazon.co.uk, Smashwords.comand other online retailers, or can be ordered from bookshops and libraries. A selection of comments from readers:
A wonderful book which I learnt a lot from as well enjoying immensely.
Both intriguing and unusual. I could hardly wait for the story to unfold as family secrets, crime and murder came to light – the ending was totally unexpected. An absorbing read.
I couldn’t put it down. I was wondering about the twists and turns all the way through. I’m not a cat person and thought I was going to be put off by all the cats, but no …
The way the story was told from all the characters’ personal viewpoints made the story deeper and more exciting. The twist at the end was great.
Well done, it was superb. Great twist that you didn’t really guess.
A revelatory read.
I loved it! I really liked the characters and the sense of buried secrets gradually coming to light. And the twists were excellent, very clever!
Loved your book. Enjoyed it right to end (including ending).

